Primary Cleft Lip and Palate
•David S. Precious, DDS, M.Sc., FRCD(C)•
© J Can Dent Assoc 1999; 65:279-83
[Primary Cleft Lip| Primary Cleft Palate |The Cleft Alveolus |CDA Resource Centre| References]
Meaningful correction of the cleft lip can be achieved only when the surgeon fully appreciates both the normal and the pathological spatial relationships and functions of the anatomic elements, particularly the muscular elements, which cause the deformity (Fig. 1). The treatment goal is to obtain morpho-functional balance between the soft tissues and the skeleton, not only by re-establishing normal insertions of all the nasolabial muscles but also by restoring the normal positioning of all of the other soft tissues, including the mucocutaneous elements.
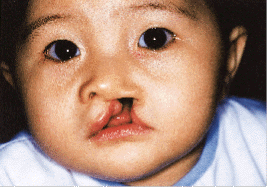 |
| Fig. 1: Unilateral complete cleft lip and palate in a 6-month-old baby. |
If, after primary surgery of the lip, oral-labial dysfunctions exist, they will exert their nefarious influences throughout a child’s growth and will lead to long-term dento-facial imbalances, some of which can be considerable.1 Thus, no matter what the initial esthetic result of the primary surgery, it is essential that the dentist conduct the most rigorous surveillance of operated patients to maintain an index of suspicion. The dentist will then be able to identify and correct any existing dysfunction as early as possible and by the most appropriate means.
Among the surgical means at our disposal are secondary functional cheilorhinoplasty, alveolar bone grafting, functional genioplasty and orthognathic surgery, the goals of which are to improve occlusion, nasal respiration, labial and labiomental function, and global facial harmony. This paper reviews some aspects of primary cleft surgery that will affect the future dental care of these young patients.
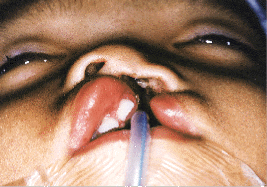
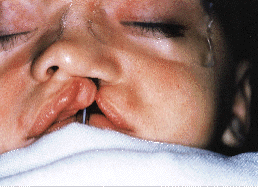
Surgery should reconstruct both the form and the function of the divided face such that balanced growth of the facial skeleton can take place. A sound knowledge of the initial faults and their post-operative sequelae enables the clinician to adapt techniques according to the needs of each case. The primary surgical procedure, performed when a child is 3 to 5 months old, is designed to systematically correct the abnormal anatomy. To correct the nasal deformity, the surgeon must obtain an ascension of the lower lateral cartilage with projection of the dome and an axial rotation of the lateral crus. In primary surgery, mucosal incisions must be short to prevent nostril constriction secondary to scar contraction, and for this reason the blind subcutaneous dissection must be both delicate and accurate. Muscle suturing is done in two planes: deep and superficial. Once these fundamental relationships have been surgically created, their maintenance can be assured with the use of a silastic intranasal retainer, stabilized by stay sutures for the first week after surgery. After that week, the retainer can be removed, cleaned and replaced in the nose on a regular schedule for 10 to 12 months. The nasal retainer has proven to be very useful in maintaining anatomical corrections achieved through functional cheilorhinoplasty (Figs. 2a and 2b). In our experience, both nasal airway patency and nostril symmetry are improved through the use of the nasal retainer (Figs. 3a and 3b).
 |
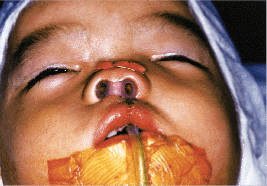 |
| Fig. 2a: Primary lip-nose surgery, before operation. | Fig. 2b: Primary lip-nose surgery, after operation. Note nasal retainer in place. |
 |
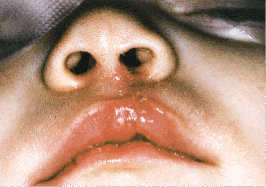 |
| Fig. 3a: Distorted anatomy before operation. | Fig. 3b: Normal anatomy restored and retained by accurate lip-nose muscle surgery. |
Primary Cleft Palate
There are three distinct regions of the mucoperiosteum covering the palate: (1) the palatine region — the thin, smooth lining covering the middle and posterior parts of the vault, corresponding roughly to the dimensions of the overlying nasal floor; (2) the maxillary region — the thick lining that covers the palate between the palatine and gingival regions, has rugae and is rich in blood vessels, nerves and connective tissue; and (3) the gingival region — the region that is intimately related to the maxillary dentoalveolus. It is the thick, maxillary mucoperiosteum, so important in the transverse and vertical growth of the palate, with which the surgeon must take special care in surgery of the hard palate.
In total bilateral cleft palate, the palatine part is missing but, usually, the gingival and maxillary regions are essentially normal. This explains why, in unoperated bilateral cleft palate, the development of the palatal vault is almost normal, the exceptions being the vomer and the palatine shelves themselves.
In classical palatorrhaphy techniques, large, widely undermined flaps of the maxillary region are swung medially to cover the defect of the palatine part. The resulting bilateral donor areas of exposed bone eventually undergo wound contraction and scarring. From its new position, the displaced maxillary mucoperiosteum cannot play its important role in transverse and vertical growth of the palatal vault. Furthermore, because this tissue is thick (unlike the thin palatine mucoperiosteum that is normally situated here), there is a "filling in" effect, which further compromises the depth of the palatal vault. The nasal fossae, normally under the influence of the palatine region of mucoperiosteum, do not fully develop their transverse dimension, which in turn can affect nasal airway patency.
It is also common in classic palatorrhaphy to obtain the nasal layer of the two-layer closure through the use of flaps of vomerine mucosa. This technique establishes an insufficient vertical dimension of the maxilla and therefore also of the nasal fossae, the net result of which favours a vertically deficient, retrodisplaced maxilla and overclosure of the mandible.2
In total unilateral cleft palate, the same problems exist with classic palatorrhaphy as in the bilateral case, except that because the vomer is bent to the non-cleft side, the transverse and vertical growth distortions are compounded by dysymmetry.
Staging of the surgical procedures based on variations of the individual case should be planned such that it is possible to respect the principles of anatomy and physiology of the three regions of mucoperiosteum that cover the palate. In complete cleft lip and palate, the soft palate is closed at the same time as the cleft lip at about 3 to 5 months of age (Fig. 4). The surgical goal is to establish both the continuity and the function of the muscles of the soft palate.
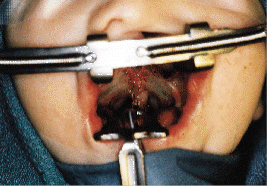 |
| Fig. 4: Soft palate muscular repair at the same time as primary lip surgery at 5 months of age. |
Adequate length of the soft palate can be achieved without either complex multiple Z-plasties or micro-surgical techniques. Incisions are made on the margins of the cleft of the soft palate, slightly favouring the nasal side. To obtain the best exposure of the levator muscle, which is retracted toward the nasal side, a small triangle of mucosa is excised from the nasal surface of the divided velum on both sides. Reconstitution of the levator veli palati as well as the palatopharyngeus and palatoglossus muscles is prerequisite to obtaining adequate soft palate length. Adequate soft tissue mobilization can easily be realized by meticulous muscle dissection. The tensor palati and superficial portion of the palatopharyngeus muscles are freed from the posterior border of the palate so that their orientation from longitudinal to transverse can be accomplished. Muscle reconstruction, including the palatoglossus, establishes a functional sphincter of the soft palate. No vomer flap is employed.
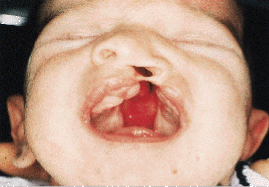
Following closure of the soft palate and the cleft lip, there is function both anteriorly and posteriorly, which causes the distance between the hamular processes, tuberosities and divided hard palate to dramatically diminish by the time the child is about 12 months (Figs. 5a and 5b). The residual hard palate cleft can then be closed, very often without the use of lateral palatal incisions. Again, no vomer flap is used because the nasal side of the cleft is closed using nasal mucosa situated below the inferior border of the vomer.3
 |
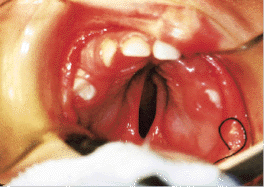 |
| Fig. 5a: Wide cleft palate, before operation. | Fig. 5b: Wide cleft palate narrows after surgery sufficiently to allow closure of hard palate with no vomer flap. |
Isolated cleft palate, both hard and soft, is treated at about 9 months of age.4 The same fundamental principles are employed in revision surgery to obtain lengthening and improved function of the soft palate.
Primary, early (within the first 18 months of life), autogenous bone grafting in reconstruction of clefts of the palate and alveolus has been demonstrated in most treatment centres to fall short of desired therapeutic results. Even when the technique used avoids disruption of vomerine mucosa, the quantity of bone present at the times of eruption of the maxillary permanent incisor and canine teeth is simply insufficient. It is generally agreed that these bone grafts do not preclude the need for early secondary alveolar bone grafts.
After conventional primary closure of a cleft lip there is inevitable scar tissue, oral nasal fistula, inadequate support for the ala of the nose and absence of bone in the region of the future permanent lateral incisor and canine teeth. The goals of secondary alveolar bone grafting (performed at about 5 to 6 years of age) are:
- closure of vestibular and palatal oral nasal fistulae
- provision of bone of sufficient quantity and appropriate quality to allow eruption of the permanent lateral incisor (if present) and canine teeth
- provision of support for the lateral ala of the nose and the skeletal nasal base
- provision of suitable bony architecture of the premaxilla and the anterior face of the maxilla on the cleft side to support accurate nasolabial muscle reconstruction
- establishment of a functional nasal airway on the cleft side.
The success of secondary alveolar bone grafts is, to some extent, time dependent. If the bone graft is performed before eruption of the permanent canine tooth, the result is almost always successful.
The criteria of success are:
- the long-term preservation of alveolar bone stock
- the eruption and periodontal health of the permanent central incisor, lateral incisor and canine teeth
- an adequate width of attached gingiva in the region of the cleft
- the absence of exposed cementum on teeth adjacent to the cleft
- the absence of oral nasal fistula.
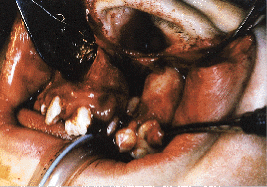
The graft material of choice is autogenous cancellous marrow of the ilium (iliac crest bone graft). This marrow is packed into the alveolar cleft defect, the soft tissue margins of which are concomitantly repaired surgically (Figs. 6a and 6b). These soft tissue margins are the palatal mucoperiosteum, the nasal mucosa and the attached and unattached buccal, vestibular gingiva.
 |
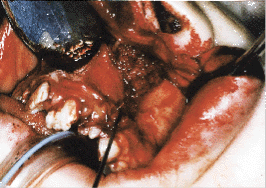 |
| Fig. 6a: Alveolar cleft defect | Fig. 6b: Alveolar bone graft in place before soft tissue closure. |
The erupting tooth stimulates alveolar and graft bone growth, and, in the vast majority of cases in our clinical experience, the canine tooth spontaneously erupts through the graft to assume a functional final position in the maxillary dental arch.
If the bone graft is delayed until the child is 8 or 9 years of age, the maxillary central incisor will already have erupted (at approximately 6 years of age), which carries the risk of periodontal bone loss and root resorption. For this and other reasons, the most appropriate time to perform alveolar cleft bone grafting is when the child is about 5 to 6 years of age.
Alveolar bone is differentially responsive in such situations because it has a distinctive physiology, reflecting its separate developmental origin from the bone that constitutes the bulk of the mandible. Alveolar bone is derived from the dental primordium, the dental papilla; its affiliation is therefore with odontoblasts, which deposit dentin.5 Alveolar bone is much more dependent on mechanical stimuli for maintenance than is bone of the body of the mandible. When teeth are removed, alveolar bone is lost very rapidly; without the mechanical stimulation provided by tooth movement, alveolar bone cannot be maintained. Alveolar bone also turns over much more rapidly than does bone of the body of the mandible.
For unilateral clefts, we perform concomitant nasolabial muscle surgery to establish midline symmetry of the face, maxilla, mandible and cranium. In bilateral cases, we perform the alveolar cleft grafts before orthodontic arch expansion; it is not prudent to perform concomitant nasolabial muscle surgery because of the risk of vascular compromise to the premaxilla.
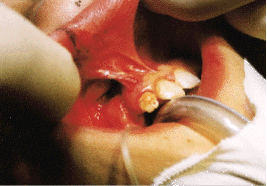
Whether bilateral or unilateral, when appropriate grafting and soft tissue procedures accomplish almost normal anatomic reconstruction of the cleft defect (Figs. 7a and 7b), there is usually significant improvement in growth, function and esthetics.
 |
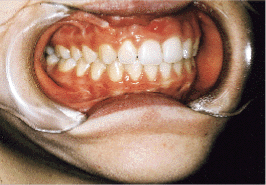 |
| Fig. 7a: Clinical appearance before alveolar bone graft and lip-nose revision to close vestibular oral nasal fistula. | Fig. 7b: Completed result after bone graft, lip-nose surgery and orthodontic treatment. |
CDA ResourceCentre
The Resource Centre has several books and information packages on cleft palate and its treatment. We also have a variety of journals and textbooks to help readers learn more about the subjects covered in this issue of JCDA.
The CDA Resource Centre, supported in part by the Dentistry Canada Fund, offers several services, including Medline searches and interlibrary loans. For more information about our services, contact the Resource Centre staff at: 1-800-267-6354, ext. 2223, or e-mail us at: info@cda-adc.ca
Dr. Precious is professor of oral and maxillofacial surgery at Dalhousie University in Halifax, Nova Scotia.
Reprint requests to: Dr. David S. Precious, Dalhousie University, Faculty of Dentistry, Oral and Maxillofacial Surgery, 5981 University Ave., Halifax NS B3H 3J5.
The views expressed are those of the author and do not necessarily reflect the opinion or official policies of the Canadian Dental Association.
References
1. Precious DS, Delaire J. Surgical considerations in patients with cleft deformities. In: Bell WH, editor. Modern practice in orthognathic and reconstructive surgery. Philadelphia, PA: Saunders; 1992. Vol. 1, Ch. 14.
2. Delaire J, Precious DS. Avoidance of the use of vomerine mucosa in primary surgical management of velopalatine clefts. Oral Surg Oral Med Oral Pathol 1985; 60:589-97.
3. Delaire J, Precious DD. Influence of the nasal septum on maxillonasal growth in patients with congenital labiomaxillary cleft. Cleft Palate J 1986; 23:270-7.
4. Precious DS, Delaire J. Clinical observations of cleft lip and palate. Oral Surg Oral Med Oral Pathol 1993; 75:141-51.
5. Precious DS. Craniofacial growth and development. In: Peterson L, editor. Principles of oral and maxillofacial surgery. Toronto: Lippincot; 1992.