• Chris L. Bryant, B.Sc., DMD •
© J Can Dent Assoc 1999; 65:566-9
[Hidden Decay - The Clinical Impasse |Air Abrasion Variables|Clinical Tips|Clinical Cases|Conculsion |References]
Traditional non-destructive methods of diagnosing pit and fissure caries, such as explorers and radiographs, have limited use in the detection of both early lesions and lesions extending well into dentin.1-3 Furthermore, bacteriological sampling of early dentin lesions provides little reason to believe that we can effectively “seal in” decay when present.4,5 With the emergence of pit and fissure decay as the most prevalent form of new decay in our population, accurate diagnosis and early prevention are becoming increasingly important. This article presents the clinician with a treatment technique for this hidden decay, which is estimated to affect 15% of first and second molars in 6- to 18-year-olds.6
Hidden Decay - The Clinical Impasse
Pit and fissure decay comprises nearly nine-tenths of new decay in children and young adults,7 despite the availability of fluoride.8,9 The decline witnessed in proximal and smooth surface caries has not been evident in fissure decay. While morphology and fluoride concentration in fissure enamel play significant roles in lowering the predisposition to gross decay, the role of fluoride in slowing established dentin caries is highly questionable.10 Any clinical efforts aimed at remineralizing early lesions must therefore differentiate between enamel lesions (successful) and lesions affecting dentin (unsuccessful).
The diagnosis of caries extending into dentin, by means of probing alone, has high specificity, but low sensitivity.11 This suggests that the majority of clinicians would agree as to what constitutes an established pit and fissure lesion, but would differ considerably on early diagnostic and treatment for small, slow-growing lesions. Faced with this impasse,12 dentists have traditionally adopted one of two treatment philosophies — either they treat or they watch.
Is there a risk in not treating these lesions? Does short-term underdiagnosis lead to long-term misdiagnosis and eventual overtreatment? While the long-term benefits of non-treatment are open to discussion,13 the long-term success of conservative intervention — whether in the form of sealants14 or minimally invasive procedures15 — is undeniable. As such, air abrasion tooth preparation is optimally suited for long-term patient benefits.
Air abrasion units allow the clinician to focus a stream of aluminum oxide particles on a specific area of the tooth. The restorative capabilities of this technique are wide-ranging and dependant on how the operator controls the following variables.
Pressure
While most available units operate between 40 and 140 p.s.i., the lowest effective pressure should be used to achieve the desired tooth preparation. For fissure surface cleansing prior to sealant application, a brief exposure at 40 p.s.i. is sufficient, while more extensive decay removal may require nozzle pressures of 80 p.s.i or more.
Tip Size
 |
| Figure 1: Air abrasion handpiece. |
Tip aperture ranges from 0.015” to 0.027” in diameter. Large tips allow more particles to pass through and are well suited for more substantial preparations, while smaller tips are best suited for discrete applications such as preventive resin restorations.
Tip Angle
Given that the angle of incidence affects the ease of preparation, manufacturers have responded with a variety of tip shapes. The handpiece tip can range from 40ş to 120ş, allowing access to both straight occlusal surfaces and the distolingual grooves of upper molars. Figure 1 shows a handpiece with a 90ş tip.
Tip Distance
By keeping the tip less than 2 mm from the target surface, the clinician maximizes the focus of the abrasive stream. Any further and the particles lose both pressure and organization, resulting in a loss of cutting ability.
Dwell Time
The longer the exposure, the further the preparation will advance. It is advisable to ensure good visual access and to confirm frequently the extent of tooth preparation, as the tactility associated with conventional rotary handpieces is absent.
Particle Size
While 27 µ aluminum oxide powder is the norm for intraoral preparation, some units are capable of carrying the much larger 50 µ powder. In my opinion, it is best to reserve the larger powder for extraoral endeavors due to its excessive cutting and the difficulty in controlling overspray.
There are clinical protocols that can help dentists successfully integrate air abrasion into their daily routine.
Case Selection
While patient involvement and cooperation contribute greatly to the clinician’s ability to offer a “no anesthetic” filling, case selection should be based primarily on the extent of the decay. For example, traditional anesthetic and rotary burs should be used for extensive dentin caries or a symptomatic tooth to ensure the patient has a comfortable experience and a restoration free of residual decay.
If using air abrasion on a tooth where dentin may be encountered, inform the patient that most people feel a slight “cool” sensation when the air abrasion particles finish removing the decay and contact the sound tooth (i.e., affected, vital, bondable dentin). On rare occasions, one may need to provide local anesthetic if the experience is not to the patient’s liking or if the clinical decay is greater than anticipated.
Rubber Dam
When moisture control and safe isolation are issues, a rubber dam must be applied for patient protection and adhesive integrity.16 Even if no local anesthetic is used, a skilled dental team can still apply a rubber dam retainer if an intrasulcular liquid topical anesthetic is delivered to the depth of the junctional epithelium with a disposable brush applicator.
Powder Control
A variety of dry suction systems that help control harmless overspray are available, but I prefer to use a modified central vacuum system. Attention to tip angle and suction position is critical to maximize evacuation effectiveness.
Restorative Material Selection
Adhesive restorative materials should be selected carefully. Flowable composites may be considered for restoring minimally prepared enamel surfaces (preventive resin restorations) if occlusal contacts are generally avoided. Otherwise, conventional microhybrids can be used when larger restorations exceed the limitations of flowable composites.
The following three cases are representative of a typical application of air abrasion to pit and fissure surfaces in children and young adults. Keep in mind that many cases may require simultaneous application of all three treatments to meet a tooth’s complete restorative needs.
Case 1: Pit and Fissure Sealant
The importance of managing susceptible fissure systems properly cannot be overstated. Our first efforts must provide successful and predictable outcomes. Sealant retention rates, if used as an indicator of long-term success, vary in the reported literature. A loss of sealant integrity of 5 to 10% per year seems to be the clinical norm.17 Possible causes for this loss include inappropriate case selection or inadequate cleansing and etching of the fissure enamel.18
 |
 |
| Figure 2: Susceptible fissures. | Figure 3: Sealant placed. |
>
Figures 2 and 3 show susceptible morphology on the mandibular premolars of a pre-teen patient requiring sealants. After ensuring no clinical decay was present, a brief pass over the fissure surfaces removed plaque and other organic matter that might have hindered etching and bonding of a visible light-cured sealant material. Cotton roll and saliva ejector control of moisture in such cases is adequate only if sustained isolation is achievable. Otherwise, consideration should be given to the use of auxiliary isolation techniques to ensure the quality of the adhesive effort.
Case 2: Preventive Resin Restoration
Where unsound enamel must be removed from a fissure system, a preventive resin restoration (PRR) can can be done. This procedure involves minimal tooth preparation followed by application of a bonding agent and an adhesive restoration.
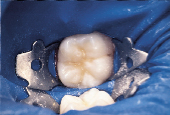
Figure 4 shows a mandibular second molar where explorer “catch” suggested that sealant application alone may have been an inappropriate treatment choice due to early enamel demin eralization. A decision to selectively remove enamel of questionable quality was made (Fig. 5) and a fourth-generation bonding agent was applied. The restorative material selected was a flowable microhybrid (Fig. 6). No local anesthetic was used other than the intrasulcular application of topical anesthetic to facilitate rubber dam placement.
 |
 |
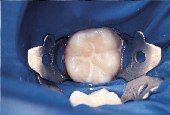 |
| Figure 4: PRR indicated - clinical “catching” on probing. | Figure 5: Unsound enamel removed. | Figure 6: Flowable composite placed. |
Case 3: Composite Resin Restoration
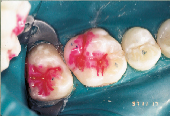
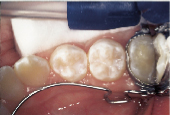
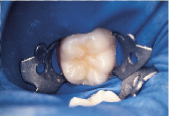
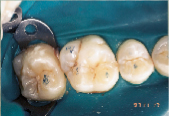
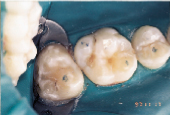
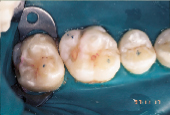
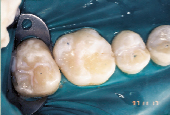
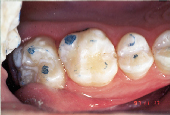
Anticipation of clinical decay extending into dentin with a resulting larger outline form requires consideration of conventional microhybrid composites. Given the concern for occlusal relationship, contacts were identified prior to rubber dam isolation (Fig. 7). Once demineralized enamel had been removed (Fig. 8), exposing decayed dentin, a caries detection dye was applied (Fig. 9) and rinsed off after 15 seconds. Infected dentin (unsound) could thus be differentiated from affected (sound) dentin (Fig. 10). A dentin bonding agent was applied and a microhybrid composite placed (Figs. 11 and 12). (Note the discrete nature of air abrasion tooth preparation, with the initial articulating paper markings remaining intact throughout the procedure.)
 |
 |
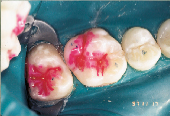 |
| Figure 7: Decay evident on maxillary first molar. | Figure 8: Demineralized enamel removed. | Figure 9: Caries detection dye placed on exposed dentin. |
 |
 |
 |
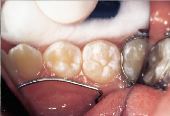
| Figure 10: Decayed dentin identified for removal. | Figure 11: Tooth restored with conventional microhybrid composite. | Figure 12: Occlusal relationship. |
While the validity of caries detection dye in identifying carious dentin is well documented, its application to enamel is unfounded and will result in false positive findings, as seen on the transverse ridge of the second molar in Fig. 10. A sealant and a preventive resin restoration was only indicated for neighbouring teeth in this case.
This restoration of a maxillary first molar was done without local anesthetic and took about 15 minutes to complete once the rubber dam was in place.
A key factor in diagnosing pit and fissure decay is recognizing the importance of early detection, and either prevention or treatment of these often small and difficult to detect carious lesions. Air abrasion preparation gives the dental team unequaled flexibility in the treatment of such surfaces.
Future improvements in the field of pit and fissure decay are much anticipated. Research into the complexity of fissure system anatomy is required, as are large-scale clinical evaluations of materials and techniques for the management of the early caries lesion. Material improvements, such as bond-assisted sealants and reduced polymerization shrinkage of sealant material, may further reduce sealant failure. Improved detection of subocclusal decay by laser fluorescent devices would be desirable.
Finally, the presumption that minimally invasive preventive measures are applicable only to children and teens must be eliminated. The financial benefit, to our patients and third-party insurers alike, of extending these services beyond the teenage years is undeniable.19
Dr. Bryant maintains a private practice in Sooke, B.C.
Reprint requests to: Dr. Chris L. Bryant, 6588 Sooke Rd., Box 951, Sooke, BC V0S 1N0
The author has no declared financial interest in any company manufacturing the types of products mentioned in this article.
1. Lussi A. Comparison of different methods for the diagnosis of fissure caries without cavitation. Caries Res 1993; 27:409-16.
2. Penning C, van Amerongen JP, Seef RE, ten Cate JM. Validity of probing for fissure caries diagnosis. Caries Res 1992; 26:445-9.
3. Weerheijm KL, Groen HJ, Bast AJ, Kieft JA, Eijkman MA, van Amerongen WE. Clinically undetected occlusal dentin caries: a radio graphic comparison. Caries Res 1992; 26:305-9.
4. Weerheijm KL, de Soet JJ, van Amerongen WE, de Graff J. Sealing of occlusal hidden caries lesions: an alternative for curative treatment? ASDC J Dent Children 1992; 59:263-8.
5. Weerheijm KL, Kreulen CM, de Soet JJ, Groen HJ, van Amerongen WE. Bacterial counts in carious dentine under restorations: 2-year in vivo effects. Caries Res 1999; 33:130-4.
6. Weerheijm KL, Gruythuysen RJ, van Amerongen WE. Prevalence of hidden caries. ASDC J Dent Child 1992; 59:408-12.
7. Brunelle JA. Oral health of United States children. The national survey of dental caries in U.S. school children; 1986-87. In: National and regional findings. U.S. Department of Health and Human Services, 1989; NIH Publication No. 89:2247.
8. McDonald SP, Sheiham A. The distribution of caries on different tooth surfaces at varying levels of caries — a compilation of data from 18 previous studies. Community Dent Health 1992; 9:39-48.
9. Weerheijm KL, Kidd EAM, Groen JH. The effect of fluoridation on the occurrence of hidden caries in clinically sound occlusal surfaces. Caries Res 1997; 31:30-4.
10. Pearce E, Larsen M, Coote G. Fluoride in enamel lining pits and fissures of the occlusal groove-fossa system in human molar teeth. Caries Res 1999; 33:196-205.
11. Tveit AB, Espelid I, Fjelltveit A. Clinical diagnosis of occlusal dentin caries. Caries Res 1994; 28:368-72.
12. Liebenberg WH. The fissure sealant impasse. Quintessence Int 1994; 25:741-5.
13. Sheiham A. Impact of dental treatment on the incidence of dental caries in children and adults. Community Dent Oral Epidemiol 1997; 25:104-12.
14. Simonsen RJ. Retention and effectiveness of dental sealant after 15 years. JADA 1991; 122:34-42.
15. Metz-Fairhurst EJ, Adair SM, Sams DR, Curtis JW, Ergle JW Jr., Hawkings KI, and others. Cariostatic and ultraconservative sealed restorations: nine-year results among children and adults. ASDC J Dent Children 1995; 62:97-107.
16. Liebenberg WH, Crawford BJ. Subcutaneous, orbital, and mediastinal emphysema secondary to the use of an air-abrasive device. Quintessence Int 1997; 28:31-8.
17. Feigal RJ. Sealants and preventive restorations: review of effectiveness and clinical changes for improvement. Pediatr Dent 1998; 20:85-92.
18. Futatsuki M, Kubota K, Yeh Y, Park K, Moss SJ. Early loss of pit and fissure sealant: a clinical and SEM study. J Clin Pediatr Dent 1995; 19:99-104.
19. Stahl JW, Katz RV. Occlusal dental caries incidence and implications for sealant programs in a US College student population. J Public Health Dent 1993; 53:212-8.