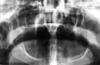
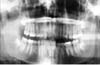
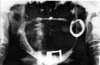
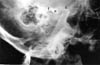
Chronic Mandibular Dislocation: The Role Of Non-Surgical and Surgical TreatmentMarco F. Caminiti, B.Sc., DDS Although the management of acute dislocations of the temporomandibular joint (TMJ) has not changed significantly in recent years, chronic dislocations continue to be treated by a variety of methods. Long-standing cases are the most difficult and frustrating to manage. This paper reports on four cases demonstrating the signs and symptoms associated with some forms of chronic TMJ dislocations, and the difficulties encountered in the management of some of these conditions. An algorithm based on a critical review of the literature is proposed for the management of both acute and chronic TMJ conditions, and recommendations are made on how to eliminate or reduce their recurrence. Introduction | Case 1 | Case 2 | Case 3 | Case 4 | Non-Surgical Management Of Mandibular Dislocations | Surgical Management | Surgery That Limits the Condylar Path | Surgical Techniques That Enhance the Condylar Path | Mandibular Dislocation: Etiologic Factors | Summary | Acknowledgments | References ] Some confusion exists regarding the meaning of the terms subluxation and luxation, or true dislocation. A subluxation is a self-reducing, incomplete dislocation of a joint in which the patient is able to close his or her mouth without assistance.1-4 Habitual subluxation is another frequently used term. It describes an often painful condition affecting normal joints, in which the condyle may be displaced anterior to the articular eminence of the temporal bone. This condition is also self-reducing.5,6 When these subluxations are asymptomatic, they should be viewed as variants of normal.7 A true dislocation (or luxation) is a condition in which a joint is displaced from its articulations and requires manipulation by another individual to return to its normal position. Manual (closed) or surgical (open) manipulation may be required to reduce the disloca- ted condyle. These temporoman- dibular joint (TMJ) dislocations may be further subdivided into acute conditions and chronic recurrent or chronic persistent dislocations. Subluxation and dislocation may be indistinguishable radiographically. In classic cases, the condylar position is anterior to the articular eminence when the mouth is opened wide. This radiographic observation is sometimes referred to as elapsio prearticularis, a term used to describe an obstructed, painless subluxation that ultimately reduces to a normal condyle-fossa relationship.3,6,8 Studies show that the condyles' range of motion is variable, and not necessarily limited to the confines of the fossa. Ricketts found that 65 per cent of normal patients were able to subluxate their condyles.9 Another study on 100 normal patients noted that 85.3 per cent of their condyles were either at or anterior to the eminence when their mouth was open to 35 mm.10 A significant difference in some cephalometric measurements as well as excessive sagittal condylar movements were seen when cephalograms were evaluated in both normal controls and patients with subluxation.11 The height of the eminence has been shown to be higher in subluxated or dislocated joints than in normal controls, however.12 It is clear from the literature that there is no standard method of evaluating or treating these TMJ conditions. This is probably due to the high success rates achieved in the management of acute conditions, and the rarity of chronic conditions. This paper describes four case reports of chronic TMJ dislocation, and proposes an algorithm for the management of these troublesome conditions. A 73-year-old woman was referred by her dentist for investigation of her abnormal bite. According to her interpreter, the malocclusion had been present for 10 years and had made her unable to chew properly. The woman was small and frail. Clinical examination revealed that she wore complete maxillary and mandibular dentures, which were maloccluded in posterior cross bite resulting in moderate facial asymmetry. Panoramic radiographic examination showed a complete dislocation of the right TMJ (Fig. 1). Fig 1: Panoramic radiograph of a 10-year dislocated right condyle. The patient was admitted to hospital, where closed reduction was attempted unsuccessfully under general anesthesia. The right TMJ was then exposed to direct vision using a traditional pre-auricular approach. It was observed that the mandibular condyle had developed a pseudoarticulation anterior to the articular eminence of the temporal bone, which was enveloped by dense fibrous connective tissue. The fibrous tissue was excised, the pseudoarticulation disengaged, and the condyle was reduced to its normal position in the glenoid fossa. Because of the patient's frail condition, maxillomandibular fixation (MMF) was not applied and a jaw supporting bandage was placed. When the patient was seen the following morning, the dislocation had recurred. The patient refused further treatment. A 16-year-old girl tripped and fell in a basketball game, striking the left side of her face against the team bench. In spite of the immediate facial asymmetry (Fig. 2) and abnormal bite that followed, the diagnosis of a dislocation was not made for two years. This was subsequently confirmed with panoramic radiography (Fig. 3). Because of the chronic nature of this dislocation, it was felt that closed reduction would probably be unsuccessful. Preparations were therefore made for open reduction through a preauricular approach. However, after the induction of general anesthesia and deep muscle relaxation, the mandible was readily reduced by closed manipulation and the jaws were immobilized with MMF in centric occlusion for 14 days. At the two-month follow-up examination, the condition had not recurred. Chronic recurrent subluxation of the right TMJ was confirmed with panoramic radiography (Fig. 4) in a 77-year-old woman with a five-year history of this condition. The right condyle assumed a position anterior to the articular eminence each time the patient opened her mouth and remained in this position unless the patient "wiggled" and/or manipulated her mandible to achieve closure. Allegedly, the onset of the condition was spontaneous. There was no relevant history of precipitating factors such as trauma or the consumption of drugs with extrapyramidal effects. The treatment plan presented to the patient included closed reduction with MMF for 14-21 days. If this proved unsuccessful, open reduction with eminectomy and MMF would be carried out. The patient refused any non-surgical or surgical treatment options, and has not been seen since her initial appointment. A 45-year-old woman who had fallen four months previously was unable to close her mouth since the accident. She had undergone several unsuccessful attempts to reduce her dislocation. Her past medical history was unremarkable. On examination, an anterior open bite of 24 mm and a restricted range of mandibular motion were observed. The patient was partially edentulous. There was a notable preauricular depression in the region of both temporomandibular joint fossae. Panoramic radiograph revealed a bilateral TMJ dislocation. Transcranial radiographs were used to demonstrate the degree of dislocation (Figs. 5a, b).
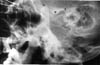
Figs 5: Transcranial radiographs of a 45-year-old woman with a four-month history of a mandibluar dislocation (Case 4). The left and the right TMJ are severely dislocated.(c: condyle, e: eminence, f: fossa). The initial attempt at manual reduction was unsuccessful. Consequently, local anesthetic was injected into one joint, around the capsule, and into the lateral pterygoid, temporalis, and masseter muscle insertions. Manual reduction was attempted again, but was unsuccessful. The contralateral side was then anesthetized, but further attempts at reduction were not successful. The patient was then sedated with demerol and diazepam, but reduction was still not obtained. Under general anesthesia with deep muscle relaxation, further attempts at closed reduction using considerable force were undertaken without success. Finally, the right TMJ was surgically explored via a preauricular incision, and the glenoid fossa, zygomatic arch and temporal fossa were exposed. Using bone hooks and Bristow elevators, followed by eminectomy and fossa debridement, unsuccessful attempts were made to torque the condyle back into place. The left side was then approached in a similar sequence. Lastly, arch bars were placed and, with a combination of maxillomandibular traction and bilateral manipulation with hooks and elevators, the condyles were reduced into their normal position. MMF was maintained for five weeks and at the one-year follow-up exam the patient was symptom free. Non-Surgical Management Of Mandibular Dislocations TMJ dislocations occur frequently as a result of protrac- ted dental procedures, blows or trauma to the mandible, bronchoscopy,13 anesthetic procedures,14,15 yawning,16-188 and drug induced19-21 or psychiatric conditions.22 The best treatment is immediate, effective reduction. Protracted and multiple attempts make further manual reductions more difficult, as the patient experiences more pain and further muscular spasm occurs. Hippocrates first described manual reduction in the fourth century B.C.23 Ambroise Pare (1633) described the use of an object that would act as a wedge in the molar regions as the chin is elevated. In this way, the condyles are lifted off their locked position.4 The approach to the acute dislocation is outlined in Table I. Chronic or long-standing dislocations that have persisted for more than one month are difficult to reduce manually. In a review study, Gottlieb24 found that only three of 24 long-standing cases were successfully reduced by manual manipulation. Another review from 1949 to 1976 reported that four out of 24 cases of long-standing dislocations were successfully reduced manually.25 Manual reduction using the hippocratic method and a mouth gag, inserted between the molars under general anesthesia, has proven to be successful.26 Manual reduction of prolonged dislocations, up to 16 months, has also been described.27 One case involved passing a wire through the inferior aspect of the mandible to aid in posterior distraction. A variety of conservative surgical techniques have been described for reducing dislocations, including the use of a bone hook passed over the sigmoid notch4 or inserted into bur holes placed at the angles.28 A Bristow elevator placed through a temporal incision can be used to apply posterior pressure to the anterior aspect of the condyle, which may force it to move posteriorly.29 A unique approach has been reported by Rao, who reduced a chronic mandibular dislocation using archbars and posterior bite splints with strong anterior wiring and Class III vector for the posterior wires.16 Anterior and inferior mandibular traction applied with a hook in the sigmoid notch has been described in the Japanese literature.30 Adekeye25 reviewed 24 patients with long-standing dislocations of from one to 120 months in duration. Four were reduced manually, nine were reduced with open procedures, seven required condylotomies, and four had myotomies or other traction procedures. Interestingly, this article makes no reference to the common surgical approaches used by Myrhaug, Irby, Leclerc, and Dautrey, but it does emphasize the difficulties encountered in adequately reducing the condyle. Another conservative treatment modality involves the injection of local anesthetic in long-standing dislocated joints. This appears to overcome the muscle spasm that is initiated by pain producing stimuli in the region of the joint, as the anesthetic disrupts the sensory side of pain or the muscle stretch reflexes.31 A report on a 54-year-old woman with a seven-week history of dislocation, who was treated with bilateral injection of 2.0 cc of prilocaine, indicated a successful reduction after 10 minutes once the jaw was manipulated. The jaws were not immobilized, but at six weeks post-op there was no pain or recurrence.31 The surgical techniques can be divided into two categories (Figs. 5):
Various techniques have been proposed for the surgical management of TMJ, but the most common are eminectomy to free all condylar movements, as described by Myrhaug in 1951,1 and the zygomatic arch inferior downfracture to limit the condylar path, as described by Leclerc in 194332 and modified by Dautrey in 1975.2 Surgery That Limits the Condylar Path Mayer, in 1933, was the first to report the displacement of the zygomatic arch (or a segment of it) in order to obstruct the condylar path. This technique was improved by Leclerc and Girard in 1943, by placing a thicker part of the zygoma into the path of the condyle.32 They performed a vertical osteotomy of the zygomatic arch and lowered the proximal segment, which then served as an obstacle to anterior condylar excursions. In 1964, Gosserez and Dautrey described a technique for the treatment of subluxations and dislocations, which involved a posterior-anterior slanting osteotomy of the eminence, and is now commonly used.33 Successful reductions of dislocations and chronic subluxations have been reported following the use of this arch downfracturing technique.3,8,34,35 Other successful modifications of the Dautrey technique to treat mandibular dislocation have also been described.8,27,36 The use of sclerosing solutions was first described by Schultze in 1947. Hypermobility was treated by injecting sodium psylliate into the periarticular tissues bilaterally to induce periarticular fibrosis and tightening of the joint.38 Injecting 0.5 per cent sodium tetradecyl sulfate into the pericapsular area every two to six weeks to produce fibrosis and subsequent limitation in condylar movement has also been described.4 Some investigators have reported a 75 per cent success rate in treating chronic subluxations with sclerosing solutions.39 Techniques that rely on a variety of bone plates to limit condylar translation have been used succes-sfully by a number of surgeons.40-44 These techniques include the use of L-shaped stainless steel pins,40 vitallium meshes,41 and condylar prostheses.42 Myotomies have also been recommended in the treatment of dislocations.45,46 Laskin45describes a technique involving a myotomy of the temporalis muscle, performed through an intraoral incision, for the treatment of three patients with prolonged dislocations. He felt that these dislocations were prolonged due to the shortening of the temporalis muscle fibres, and that the liberation of these fibres would help reduce the dislocation. However, later results involving lateral pterygoid myotomy indicated that the use of silastic sheeting as an interpositional material did not prevent lateral pterygoid muscle reattachment, because the fibres reattached to the pseudocapsule formed around the material.4 Refinements in myotomy techniques have also been reported, with variable results, for the treatment of recurrent mandibular dislocation.46,51 Surgical Techniques That Enhance the Condylar Path Riedel, in 1883, was the first to report the surgical treatment of TMJ dislocation. His technique involved a unilateral excision of the condyle (condylectomy). It was subsequently described by Myrhaug,1 who introduced a procedure in which the entire eminence was removed to completely eliminate any interference to condylar movement. He reported on the successful treatment of two cases in 1951.1 Other surgical procedures for the treatment of recurrent dislocations have included meniscectomy48 and closed condylotomy.49,50 Tasanen and Lamberg used the Kostecka method (with a Gigli saw and no MMF) to treat 21 patients.50 Seven patients had recurrences for two years, and 14 patients had them over at least one month. At the one-year follow-up, 17 patients no longer had dislocations, two underwent a further procedure, two were unsuccessful, and one case developed a pseu-doarthrosis requiring a costochondral graft.50 In the United States, Irby popularized the same technique described by Myrhaug. He reported obtaining good results in the treatment of 30 cases.51 Critics of this procedure note that it is unphy- siologic, that the intraarticular approach may be damaging to the joint, and that zygomatic arch fractures may occur.8,47 However, very favorable results have been reported using the eminectomy technique and its variations, and good clinical outcomes have been achieved for many patients with chronic mandibular dislocation.5,29,52-55 Complete removal of the articular eminence does not lead to intracranial complications. However, since some eminences may have large marrow spaces, resulting in a potential increase in the risk of wound infection, antibiotic therapy is recommended preoperatively and postoperatively.53 Blankestijn and Boering47 reported using a modification of the Myrhaug technique with 16 patients. They did not enter the joint proper, but focused on the lateral and anterior joint regions during the resection of the articular eminence. The procedure was completed by suturing the periosteum and cartilage covering the osteotomy site. They operated on 31 joints with eight-month to nine-year follow-ups. Nine patients had no recurrences, five showed some improvement and retained the ability to subluxate, and two had no improvement, but patients subjectively felt an overall improvement. They theorized that the free movement of the condyle and postoperative scar tissue formation were the reasons for success. Although some patients had inadvertent joint penetration, there was no evidence of joint degeneration.47 Sensoz et al12 treated 39 patients with dislocation and 13 with recurrent subluxation. They are the only investigators who compared the eminence height of their study group (10.7 mm) to normal controls (7.4 mm) and found a significant difference. Surgery was carried out using a preauricular approach, and the eminence was removed with chisels. They also measured echographic changes, and found a difference between pre-operative patients and the controls, as well as between the patients preoperatively and post-operatively (i.e. joint noises). The average follow-up was 18 months, but discomfort and slight ache subsided after a few weeks. Symptoms were relieved in almost all patients, but two patients underwent the surgery again to remove more of the medial portions of the remaining eminence. All patients underwent bilateral procedures, as the authors believed that both joints would eventually become symptomatic even in the presence of unilateral dislocation.12 Mandibular Dislocation: Etiologic Factors A variety of factors have been implicated as causative agents in mandibular dislocation. These include trauma, yawning, drugs, anesthetic procedures, psychiatric disorders, muscular dyskinesias, and connective tissue disorders. Extrapyramidal side effects have been observed with certain antiemetics (metoclopramide).20 In addition, certain drugs used in the treatment of psychiatric conditions have been reported to cause extrapyramidal effects, including phenothiazines (used in the treatment of schizoprenia),57 haloperidol,19 and thiothixene.21 Several psychiatric disturbances may produce mandibular dislocations. The recurrent subluxation of the TMJ referred to by Patton as psychogenic subluxation may be the primary presenting feature of psychiatric disturbances.22 The clinical pattern of dislocation in this group of patients may be chronic recurrent or chronic persistent in nature, and unilateral or bilateral. In addition, redislocation after successful reduction is not uncommon. Dislocations may also result from dyskenesias that may be psychiatric in etiology, or due to abnormalities in the extrapyramidal system.58 Anesthetic procedures are commonly associated with dislocations. Subluxation and dislocation have been reported during induction,59 during intubation,14 and during fibreoptic bronchoscopy.13 Since the majority of these occurrences are acute in nature, immediate reduction is usually successful. Although some medical literature indicates that yawning rarely causes mandibular dislocation,17,18 this review indicates that it does so quite frequently.4,16,25,50 Patients suffering from connective tissue disorders can develop dislocations of the TMJ. A 17-year-old woman developed painful TMJs, and then one year later began to experience frequent dislocations. She also developed patellar and radio-ulnar dislocations, and was diagnosed with Ehlers-Danlos syndrome. After failed treatment (immobilization, condylotomy), she was managed with a condylectomy and elastic traction.56 Ideally, acute mandibular dislocation requires immediate effective reduction, which can usually be accomplished with a closed technique. Dislocations that persist for more than one month are classified as chronic, and although they may be effectively reduced by conservative means using traction devices, they often demand the use of adjunctive techniques, including manipulation under general anesthesia and/or surgical techniques. While successful results are usually achieved with eminence augmentation, eminectomy is equally effective and produces fewer complications. Four case reports emphasizing the unpredictability associated with the management of some patients with chronic mandibular dislocation have been presented, in addition to a review of non- surgical and surgical treatment. Dr. Caminiti is the former chief resident, department of oral and maxillofacial surgery, University of Toronto and The Toronto Hospital. He is a clinical fellow at The Centre for Research and Education, University of Toronto, Faculty of Medicine. Dr. Weinberg is a professor, University of Toronto, faculty of dentistry, department of oral and maxillofacial surgery, and staff oral and maxillofacial surgeon, The Toronto Hospital. Reprint requests to: Dr. Marco F. Caminiti, The Centre for Research and Education, U. of T. Faculty of Medicine, 585 University Ave., Toronto ON M5G 2C4.
|