

Langue percée et dent fracturée
Christine Botchway BDS, LDSRCS(Eng.), DDPHRCS(Eng.), MSC (Uni Lond)
Iris Kuc, DDS, B.Sc., PhD
SOMMAIRE
L’étude de cas dont fait rapport le présent article a pour objet de sensibiliser le public sur l’incidence de plus en plus fréquente des fractures de dent résultant du trauma occasionné par l’insertion d’une barre linguale lors du perçage de la langue. Le perçage buccal gagne de la popularité. Les professionnels de la santé s’inquičtent des risques qui y sont associés ŕ savoir, entre autres, les dommages causés aux dents, l’infection, le trouble de la parole et la lésion d’un nerf. S’y ajoute la conviction que, dans certains cas, les clients qui envisagent de se faire percer une partie du corps ne reçoivent peut-ętre gučre d’instructions sanitaires post-opératoires, les mettant ainsi ŕ plus grand risque de complications. En conclusion, une campagne de sensibilisation sur la santé publique sous forme d’activités promotionnelles et éducatives est incontournable si l’on veut assurer un perçage sécuritaire et responsable. Nous recommandons également que soient préparés des ateliers, des forums et des dépliants éducatifs ŕ l’intention des perceurs, de la clientčle et des professionnels de la santé en Alberta.Mots Clés MeSH : self-mutilation/complications; tongue/injuries; tooth fractures/etiology
© J Can Dent Assoc 1998; 64:803-5
Cet article a fait l’objet d’une révision par des pairs.
[Body Piercing and Society | Clinical Case | Risks of Intraoral Piercing | Learning More About Piercing | Recommendations | References]
Although it has an ancient history, body piercing has only recently attained popularity in Western society.1,2 For centuries, body piercing was part of many cultures and religious rites.2 Ancient Egyptians pierced their navels to signify royalty, Roman centurions wore nipple rings as a sign of virility and courage, and Mayans pierced their tongues for spiritual purposes.3 In North America, body piercing was also a tradition of the Sioux.5
Today, popular sites for body piercing include the ears, eyebrows, lips, nose, nipples, navel, penis, scrotum, labia, clitoris and tongue.4,5 Of significance to the dental community is the recent increase in intraoral piercing,4,5 which is the insertion of jewelry into soft oral tissues including the lips, cheeks and tongue.1 It is critical that the dental profession become aware of the recent interest in this type of body piercing, of the impact this trend may have on dentition and speech, and of the health risks that are associated with piercing.
The literature on the effects of tongue piercing is limited. What there is points to the risk of tooth damage, the possibility of aspiration of jewelry,4 speech modification,3 and an increased risk of infection.5 Furthermore, we suspect that body piercers do not provide sufficient health information to their clients. As a result of these findings, we present here a case of fracture and possible abrasion caused by a tongue ring in a 23-year-old Caucasian male. Although this case is not unique in its presentation, it serves to highlight for the dental profession some of the risks involved in intraoral body piercing.
A 23-year-old single male presented himself to the University of Alberta undergraduate clinic complaining of "chipped molars and some worn teeth." The patient was a transient worker for an oil company. Long hours on the job and other personal factors induced a moderate level of stress. Aside from the fact that he was a smoker, his medical history was unremarkable. His past dental history had included extractions (third molars) and dental hygiene. Current clinical findings revealed no extraoral abnormalities. The intraoral exam revealed no carious lesions and good periodontal health, with a periodontal screening record (PSR) of 2.6
However, a number of distinct fractures involving enamel and dentine were observed on the incisal edges of teeth #12 and #31 and the lingual surfaces of #36, #46 and #16.
The soft tissues were all within normal limits with the exception of the anterior central area of ventral aspect of the tongue, which appeared slightly inflamed. The patient did not reveal the use of a ring until questioned about the inflamed areas, at which time he inserted the barbell-type ring (Fig. 1).
Fig. 1: Barbell rings …a risky fashion option?
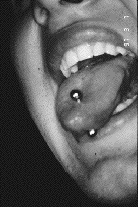
The patient also reported a tongue-thrusting habit with the additional parafunctional habits of grinding and clenching.
Upon questioning the patient as to the possible cause of the fractures, he indicated that he had obtained the ring eight months earlier and was having difficulty becoming accustomed to the presence of a foreign body in his oral cavity. The fractures had all occurred within the first month of obtaining the barbell. He also indicated some initial difficulty in speech and mastication following the piercing. Despite the patient’s parafunctional habits, he indicated that he occasionally slept with the ring inserted. We conclude that this only served to compound the risk of trauma to his dentition.
Piercing of the tongue is normally performed in the midline of the tongue anterior to lingual frenum.4 Because of the swelling, it is recommended that a longer barbell shank initially be placed in the tongue, followed by the insertion of a shorter barbell shank after healing. (Significantly, the patient had not had the initial tongue ring changed.) Because of the tongue’s vascular nature, healing is generally quick, occurring within 4 to 6 weeks after the piercing.7 The procedure is usually performed without anesthesia. The protruding tongue is clamped and supported by a piece of cork, then pierced by a needle bearing equal gauge to that of the barbell stem.4
The patient said he had his tongue pierced simply because he "wanted to." While the reasons for piercing are varied, it is generally considered either a form of body art, fashionable, a "personal statement" or daring.7 Piercings are also sought for their sexual7 and spiritual benefits.4,8 Our patient also had his nipples pierced. Both his piercings were hidden and he had removed his tongue ring prior to presenting for the oral examination. There is some suggestion that body piercing is seen as deviant behaviour by society,5 which may explain why some individuals do not always present for their dental appointments with their pierced ring in place. Piercing should therefore be included in a list of differential diagnosis for any inflamed areas of soft tissue as it may not always be readily obvious.
There are a number of risks associated with the practice of intraoral body piercing that are of concern to the dental community. They include:
1. Tooth fracture: Our clinical case serves to illustrate one of the most immediate outcomes associated with intraoral piercing. In addition, when a patient reports parafunctional habits such as bruxism, it is not unreasonable to infer that the risk of tooth fracture increases. Individuals who choose piercing need to be made aware of this risk and that damage to the dentition may result in cracked tooth syndrome or outright fracture of the dental hard tissues with or without pulpal involvement.
2. Speech impediment: A review of the literature suggests that speech may be hindered.3 In one case, a student with a pierced tongue was forced to remove his barbell because his speech was altered.3
3. Aspiration: It is not unreasonable to count as a risk the accidental aspiration of a piece of the jewelry inserted in the tongue should the jewelry come apart.4
4. Infection and allergic response: Infection from unsterilized instruments is always a risk. Body piercing is often done in the same establishments as tattoo studios.7,9 Despite performing invasive procedures, many body piercers do not have any formal education on sterilization, effective skin care and proper infection control.9 Consequently, piercing may include an increased risk of the transmission of Hepatitis B, HIV/AIDS, tetanus,6 syphilis and tuberculosis.5 The literature does not provide statistics on the risk of transmission of these diseases due to the lack of regulation on body piercing.5 Allergic reactions to nickel or other alloys used in the metals are also a possibility.7 All jewelry should be made of inert non-toxic metals7 such as stainless steel, 14K gold niobium or titanium.7 The patient reported that his barbell was made of stainless steel.
5. Other: A number of side effects associated with piercings have been documented,5 including pain, deep cyst formation, hypertrophic scarring, damage to deeper structures such as superficial veins and nerves, haematoma formation and neuroma.5 Septicaemia and toxic shock syndrome have also been reported in cases of severely infected body piercings.4 It is not unreasonable to infer that other risks specific to the practice of tongue piercing may include damaged cheek tissue, permanent numbness and loss of taste.
Many piercers are not professionals. It is suggested that in some cases, post-operative instructions are inadequate. Proper post-operative instructions should include information on the care of the pierced site; for tongue piercing, that means frequently using a mouth rinse and avoiding alcohol, spicy foods and smoking.7
It is clear from the literature that whether health professionals like it or not, body piercing will continue.9 As a result, they need to know about the procedure to be able to provide helpful information.2 Health professionals and the general public still have much to learn about the effects of tongue piercing on the integrity of dentition and speech, and the risk of infection. It is also important that they understand the motivation and feeling of gratification that compel people to choose body piercing in spite of these possible complications. Based on the literature and the case presented, it is clear that damage from such piercing should be of concern to the dental profession.
As health care professionals, we need to be aware of the procedures and risks involved in tongue piercing, and of the social and psychological reasons that lead people to engage in this practice regardless of the risks.
Hence, it is proposed that leaflets addressing the issues for both health care professionals and the public be prepared and distributed as a public health education measure. This would enable us to advise patients who may be pierced as to the procedures they should follow and the risks they may face. It is also proposed that a survey be conducted to investigate the practices of body piercers in Edmonton and the knowledge of their clients.
Dr. Botchway is teaching fellow, Oral Diagnosis, Oral Health Sciences, Faculty of Medicine, University of Alberta.
Dr. Kuc is associate professor, Oral Diagnosis, Oral Health Sciences, Faculty of Medicine, University of Alberta.
Reprint requests to: Dr. C. Botchway, Room 2089, Oral Health Sciences, Faculty of Medicine, University of Alberta, Edmonton AB T6G 2N8.
DISCLAIMER
1. Scully C, Chen M. Tongue piercing (oral body art). Br J Oral Maxillofac Surg 1994; 32:37-8. 2. Boardman R, Smith RA. Dental implications of oral piercing. Oral Health 1997; 87:23-31.
3. Armstrong ML, Ekmark E, Brooks B. Body piercing: promoting informed decision making. J Sch Nurs 1995; 11:20-5.
4. Reichl RB, Dailey JC. Intraoral body piercing: a case report. Gen Dent 1996; 44:346-7.
5. Wright J. Modifying the body: piercing and tattoos. Nurs Stand 1995; 10:27-30.
6. Rethman J, Rethman M. Periodontal screening and recording. Why, when and how. Pract Hyg 1993; 2:19-23.
7. Armstrong ML. You pierced what? Pediatr Nurs 1996; 22:236-8.
8. Armstrong M.L. What practicing R.N.s should know. Texas Nursing 70:8-10 1996.
9. Malloy D. Body piercings. In: Vale V, Juno A (eds). Research No. 12: Modern Primitives. San Francisco, Calif: Research Publications, 1989.