

Le kyste de la bifurcation buccale : le traitement non chirurgical est-il une option?
Lesley A. David, DDS
George K.B. Sŕndor, MD, DDS, FRCD(C), FRCS(C), FACS
Douglas W. Stoneman, DDS, FRCD(C)
SOMMAIRE
Le kyste de la bifurcation buccale (KBB) mandibulaire a été décrit pour la premičre fois par Stoneman et Worth en 1983. Il s'agit d'une lésion ŕ un endroit spécifique, généralement ŕ la surface buccale de la premičre molaire de la mandibule et, plus rarement, ŕ celle de la deuxičme molaire de la mandibule. La littérature offre de nombreux comptes rendus décrivant le KBB et son traitement. Jusqu'ŕ présent, le traitement préconisé comprend l'extraction de la premičre molaire atteinte ainsi que la marsupialisation et l'énucléation du kyste. Dans leur dernier article, Pompura, Sŕndor et Stoneman parlent du traitement réussi de 44 kystes avec énucléation, mais sans extraction de la dent. Cet article explique les caractéristiques diagnostiques du KBB et présente trois cas avec en tout cinq kystes qui ont été traités sans procédures chirurgicales et qui ont fini par ętre guéris. Aussi les auteurs proposent-ils de songer ŕ une méthode non chirurgicale plus conservatrice.Mots clés MeSH:mandibular diseases/pathology; molar child; periodontal cyst/pathology.
© J Can Dent Assoc 1998; 64:712-6
Cet article a fait l'objet d'une révision par des pairs.
[ Introduction | Cases | Discussion]
The buccal bifurcation cyst (BBC) is an uncommon lesion associated with the permanent mandibular first or second molar in children. Usually it is identified just prior to eruption. Stoneman and Worth in 1983 were the first to describe the lesion and report its radiographic and clinical features.1 They named the lesion mandibular infected buccal cyst. Similar lesions have been described in the literature under a variety of names. They include the circumferential dentigerous cyst,2 the inflammatory paradental cyst,3 and the inflammatory collateral dental cyst.4 The World Health Organization5 describes this lesion under the name "paradental cyst." Neville, Damm and Allen et al. state that this latter name should be avoided because it is non-specific.6 Pompura, Sŕndor and Stoneman7 argue for the term BBC, because the lesion is site- and age- specific. It has a constant relationship to the mandibular first molar's buccal bifurcation (Table I).
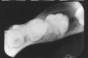
The radiographic presentation of the BBC may be subtle and easily overlooked unless the lesion is large or symptomatic. If a BBC is suspected, a panoramic or periapical radiograph should be taken as well as an occlusal film (Fig. 1).1 The BBC's distinct radiographic features are listed in Table II.
| Table II | ||||||||
| Radiographic Features of the Buccal Bifurcation Cyst | ||||||||
|
The histology of this lesion is non-specific and reveals non-keratinized stratified squamous epithelium, areas of epithelial hyperplasia and an inflammatory infiltrate in the connective tissue wall. Bacteriology reports have shown a mixed flora.7-9
The differential diagnosis of this lesion includes eosinophilic granuloma, lateral periodontal cyst, traumatic bone cyst and periostitis ossificans. Usually, the clinical and radiographic features distinguish the BBC from other conditions.8
Treatment of the BBC has evolved over time. The low incidence of this lesion makes randomized controlled trials impractical. Stoneman and Worth report successful treatment through tooth extraction and curettage of the lesion, as well as with endodontic treatment of the tooth and curettage of the lesion.1 Enucleation and extraction are reported by Trask, Sheller and Morton10 and more recently by Martinez-Conde, Aguirre and Pindborg.11 Stanback reports treatment via marsupialization.12 Enucleation alone is reported by several authors.8,9,13,14 Pompura, Sŕndor and Stoneman7 recently report the successful treatment of 44 BBCs with enucleation alone (without tooth extraction). The following cases illustrate an even more conservative approach to treatment.
Case 1
During an orthodontic consultation, an 8-year-old male was noted to have bilateral cystic lesions of the mandible. He was asymptomatic, but on intraoral examination buccal tilting of the associated teeth and deep buccal periodontal pockets were noted. Mild bilateral swelling was noted extraorally. The lesions were pointed out to the patient and his mother, who were advised to see an oral and maxillofacial surgeon for management.
The family moved away for a year and never sought treatment. At a follow-up visit 15 months later, the lesions showed definite signs of radiographic resolution. Six months after this initial follow-up, there was no clinical or radiographic evidence of the cysts at all (Figs. 2a-2f).
Case 2
A 9-year-old male had BBCs associated with teeth 3.6 and 4.6. These teeth were tilted buccally and were associated with deep buccal periodontal pockets. No treatment was rendered. During nine months of follow-up, the cyst adjacent to tooth 4.6 enlarged and required surgical treatment, and the cyst adjacent to tooth 3.6 regressed without treatment (Figs. 3a-3d).
Case 3
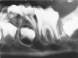
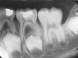
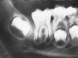
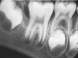
A 7-year-old male was treated by his physician with a course of amoxicillin for pain and swelling of the mandible and was subsequently referred to his dentist. On examination, the patient had swelling and tenderness in the region of the right angle of the mandible. Intraorally, the soft tissues buccal to teeth 3.6 and 4.6 were inflamed and slightly erythematous. Periodontal probing revealed depths of 11 mm to 12 mm bucally. Both crowns were tilted buccally. The pockets were irrigated with saline and hydrogen peroxide and the patient was instructed to irrigate these areas at home daily with saline rinses. The patient was reassessed weekly. Over several months, the defects resolved with irrigation and the periodontal status returned to normal. The probing depths were 2 mm to 3 mm buccally, and the patient's pain, swelling and inflammation ceased (Figs. 4a-4d).
The etiology of the BBC remains uncertain. Different theories have been proposed. During eruption, as the cusps penetrate the oral epithelium, a localized area of inflammation may occur beneath the epithelial attachment. The fact that the mesiobuccal cusp of the first molar is the first to break through the epithelium might explain the development of the lesion on the buccal surface at about the time of eruption.1 The cystic epithelium may be derived from the cell rests of Serres, the cell rests of Malassez, apical migration of cells of the dental lamina or reduced enamel epithelium.7 As Camarda, Pham and Forest8 state, however, this explanation does not account for the reason these lesions have not been seen with erupting incisors. Another hypothesis is simply that this cyst is a variant of the lateral periodontal cyst.1 This lesion is also site-specific, namely to the canine and premolar region, and rarely occurs in children.7 Enamel projections into the buccal bifurcation may also be a causative factor.
Pompura, Sŕndor and Stoneman point out that these lesions are not seen in adults and questioned whether they may be self-limiting.7 Evidence from these three patients with five cysts indicates that some of these lesions are self-limiting. The authors speculate that perhaps microtrauma and subsequent inflammation of the buccal gingival tissues and the cyst lining may induce a small opening into the lesion. This "automarsupialization" may allow the cyst to depressurize and heal spontaneously. Periodontal probing may also result in "micromarsupialization." Case 2 illustrates simultaneous regression of a lesion on one side and continued growth of a BBC on the contralateral side. Factors that predict which lesions may be more susceptible to spontaneous resolution are unknown. Although there are no guidelines on which cysts need to be watched and which require surgical treatment, the authors emphasize that at least some BBCs may not require surgery. Consideration should therefore be given to managing BBC cases conservatively with an expectant "watchful inactivity." Clinical and radiographic re-evaluation should occur at three- to six-month intervals. Infected lesions or those increasing in size must be managed surgically.
Acknowledgment: the authors thank Dr. M. Dagenais for her radiographic contribution to this paper.
Dr. David is resident, Oral and Maxillofacial Surgery, University of Toronto.
Dr. Sŕndor is coordinator of Oral and Maxillofacial Surgery, Hospital for Sick Children and Bloorview MacMillan Centre; director, graduate residency program in Oral and Maxillofacial Surgery, The Toronto Hospital; and assistant professor, University of Toronto.
Dr. Stoneman is professor emeritus, Department of Radiology, Faculty of Dentistry, University of Toronto; and consultant oral radiologist, Hospital for Sick Children and The Toronto Hospital.
Reprint requests to: Dr. G.K.B. Sŕndor, Hospital for Sick Children, 555 University Ave., Toronto, ON M5G 1X8.
Cliquez ici pour une grande image
Fig. 1: Occlusal radiograph of a buccal bifurcation cyst showing lingual displacement of the first molar roots and the resultant increased prominence of the lingual cusps. Note also the thinning of the buccal cortex and periosteal reaction.
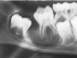
Cliquez ici pour une grande image
Fig. 2a: Large buccal bifurcation cyst around tooth 4.6.

Cliquez ici pour une grande image
Fig. 2b: Bone fill noted at 15 months without treatment.
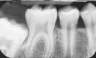
Cliquez ici pour une grande image
Fig. 2c: Complete resolution of cyst with uprighting of tooth 4.6 at 21 months.
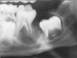
Cliquez ici pour une grande image
Fig. 2d: Lesion around tooth 3.6.

Cliquez ici pour une grande image
Fig. 2e: Bone fill at 15 months without treatment.
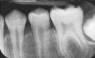
Cliquez ici pour une grande image
Fig. 2f: Complete resolution of cyst
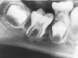
Cliquez ici pour une grande image
Fig. 3a: Lesion around tooth 4.6 with faint radiopaque concave line at apices and prominent lingual cusps.
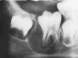
Cliquez ici pour une grande image
Fig. 3b: Spontaneous enlargement of lesion 9 months later.

Cliquez ici pour une grande image
Fig. 3c: Lesion around tooth 3.6 with faint radiopaque lines at apices and prominent lingual cusps.
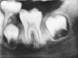
Cliquez ici pour une grande image
Fig. 3d: Spontaneous bone fill around apices and mesial and distal of tooth 3.6 at 9 months without treatment.
Cliquez ici pour une grande image
Fig. 4a: Faint radiopaque line at apices and distally around tooth 3.6.
Cliquez ici pour une grande image
Fig. 4b: Resolution of cyst at tooth 3.6.
Cliquez ici pour une grande image
Fig. 4c:Smaller cyst at tooth 4.6; faint radiopaque line at mid apices
Cliquez ici pour une grande image
Fig. 4d: Spontaneous healing of cyst at tooth 4.6..
.
References
1. Stoneman DW, Worth HM. The mandibular infected buccal cyst_molar area. Dent Radiogr Photogr 1983; 56:1-14.
2. Thoma KH. The circumferential dentigerous cyst. Oral Surg Oral Med Oral Pathol 1964; 18:368-71.
3. Craig GT. The paradental cyst. Br Dent J 1976; 141:9-14.
4. Main DMG. Epithelial jaw cysts: a clinicopathological reappraisal. Br J Oral Surg 1970; 8:114- 25.
5. Kramer IRH, Pindborg JJ, Shear M. Histological typing of odontogenic tumors. 2nd ed. Berlin: Springer-Verlag, 1992. p. 40-2.
6. Neville BW, Damm DD, Allen CM, Bouquet JE. Oral and maxillofacial pathology. Philadelphia, PA: WB Saunders; 1995. p. 74.
7. Pompura JR, Sŕndor GKB, Stoneman DW. The buccal bifurcation cyst_a prospective study of treatment outcomes in 44 sites. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1997; 83:215-21.
8. Camarda AJ, Pham J, Forest D. Mandibular infected buccal cyst: report of two cases. J Oral Maxillofac Surg 1989; 47:528-34.
9. Bohay RN, Weinberg S, Thorner PS. The paradental cyst of the mandibular first molar: report of a bilateral case. ASCD J Dent Child 1992; 59:361-5.
10. Trask GM, Sheller BL, Morton TH. Mandibular buccal infected cyst in a six-year-old girl: report of a case. ASCD J Dent Child 1985; 52:377-9.
11. Martinez-Conde R, Aguirre JM, Pindborg JJ. Paradental cyst of the second molar: report of a case. J Oral Maxillofac Surg 1995; 53:1212-4.
12. Stanback JS. The management of bilateral cysts of the mandible. Oral Surg Oral Med Oral Pathol 1970; 30:587-91.
13. Vedtofte P, Praetorius F. The inflammatory dental paradental cyst. Oral Surg Oral Med Oral Pathol 1989; 68:182-8.
14. Packota GV, Hall JM, Lanigan DT, Cohen MA. Paradental cysts on the mandibular first molars in children: report of five cases. Dentomaxillofac Radiol 1990; 19:126-32.
15. Ackerman G, Cohen MA, Altini M. The paradental cyst: a clinicopathologic study of 50 cases. Oral Surg Oral Med Oral Pathol 1987; 64:308-12.
16. Fowler CB, Brannon RB. The paradental cyst: a clinicopathologic study of six new cases and review of the literature. J Oral Maxillofac Surg 1989; 47:243-8.
17. Wysocki GP, Brannon RB, Gardner DG, Sapp P. Histogenesis of the lateral periodontal cyst and the gingival cyst of the adult. Oral Surg Oral Med Oral Pathol 1980; 50:327-34.