Resin-Metal Bonding Systems: A Review Of the Silicoating and Kevloc Systems
Randall D. Mazurat, B.Sc., DDS
Simona Pesun, B.Sc., DMD
The Silicoating and Kevloc systems are resin-metal attachment devices that are designed to improve bond strength and decrease microleakage at the resin-metal interface. Clinically, these systems can be used to place resin pontics and veneers, enhance cementation with resin cements, and bond the resin matrix to metal implant substructures. To provide practitioners contemplating the use of either modality with background information, a concise summary of the potential advantages of resin-metal bonding, the procedures required to establish the chemical bond, and the methods of evaluating laboratory studies are presented. Chemical bonding with these systems is technique sensitive. How the system is used may be as important to the final clinical results as is the choice of system.
Clinical Implications Of Resin-Metal Bonding | Advantages | Uses | What's the Clinical Relevance? | Chemical Bonding With the Silicoater MD and Kevloc Systems | Evaluating Resin-Metal Bonding Systems | Summary | Acknowledgments | References ]
Clinical Implications Of Resin-Metal Bonding
In prosthodontics, the attachment of a resin matrix to a metal framework may pose significant difficulties. The major problems are related to the strength of attachment and the space available for restorative materials. A low bond strength between the resin and metal may result in microleakage, discoloration or breakage, while a restriction in the space available to place metal, resin matrix, and denture teeth may result in compromised tooth placement and a less than ideal bond between materials. Limited space may be available for materials if the interocclusal distances are restricted. It can also be a problem when single tooth replacement or resin bonded retainers are provided. Clinically, limited space and low bond strength may result in unacceptable esthetics, a need for excessive adjustment of the occlusion, or the breakage of any of the materials. To prevent clinical problems, it is therefore imperative to optimize the strength of the resin attachment to the metal framework, and ensure that there is sufficient room for materials.
Until recently, the attachment of the resin matrix to a metal framework has been maintained primarily through mechanical retention. Mechanical retention can be achieved using latticework, mesh, beads, and various posts.1 Alternative attachment mechanisms are now available, however, including micromechanical and chemical attachment systems.
Micromechanical attachment can be accomplished using sandblasting, electrochemical etching, and chemical etching.2 Conversely, chemical attachment may be achieved using adhesive cements, porous metal coatings, tribochemical coating, Silicoating3 and the Kevloc system. These alternative attachment systems are used either as an addition to or in place of conventional macromechanical retention.
The "ideal" attachment system should produce and maintain a strong and consistent bond between the resin and metal. Our interest in new resin-metal attachment systems stems from the problems that have been experienced with macromechanical retention as well as the current resin-metal attachment mechanisms, both of which exhibit failure at the resin-metal interface.
What are potential advantages of the alternative resin-metal attachment systems?
Their manufacturers recommend that we adopt the technique of chemically bonding resin to metal, and eliminate macromechanical retention altogether, for the following reasons:
- The increase in bond strength between the resin and metal.
- The decrease in microleakage at the resin-metal interface.
- The reduction in metal impingement on the space needed to place the resin and teeth.
- The improvement in esthetics because of opaquing and increased space.
Clinically, we have been able to apply chemical bonding techniques to several procedures, including:
- Resin pontics for cast partial dentures.
- Resin veneering for conventional and implant fixed partial dentures.
- Preparation of restorations (onlays, inlays, metal retainers) prior to cementation.
- Bonding of resin matrix to the metal implant substructure.
Resin Pontics
The attachment of a single prosthetic tooth during the fabrication of a removable partial denture may pose a problem when space is restricted, or it is necessary to achieve a harmonious esthetic result with the adjacent natural dentition.
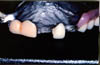
By fabricating a metal pontic in the cast framework, and then bonding a custom resin facing, it is possible to fabricate a single tooth replacement that has excellent strength and natural esthetics, and will fit into a restricted space. Many of the resin systems available today provide a wide range of shades that can be customized to blend with the natural dentition (Fig. 1). However, the resin pontic procedure is technique sensitive and more costly than the conventional procedure of attaching a denture tooth to the cast framework with acrylic resin.
Fig 1: Resin pontics for single tooth placement.
Resin Veneering
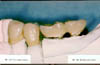
Resin can be used for both facings and occlusal surfaces as an alternative tooth colored material to porcelain (Fig. 2). The resins are less abrasive and more resilient than porcelain, and they are somewhat easier to apply, adjust and repair. If the clinician perceives these features to be important, resin veneering may provide a substitute for porcelain.
Fig 2: Resin veneers for fixed restorations.
The resin-metal fixed prosthesis also makes an excellent long-term transitional restoration when esthetics and cost are critical. However, the long-term clinical success data to support routine adoption of resin veneering are unavailable.
Restoration Preparation
Prior To Cementation:
The cementation of inlays, onlays and metal retainers with resin cements can be improved by using micromechanical or chemical systems. For example, applying the opaquing agent on the metal surface of the retainers used for Maryland bridges will mask the metallic color and may significantly improve esthetics. Not all resin-metal bonding systems are applicable to all types of metals or resins, however. Another disadvantage is that the interface layer, crucial for the bond strength, can not be altered at the try-in stage.
Bonding Of Resin To Metal Implant Substructures:
When a fixed-removable implant prosthesis is fabricated, there is often a limited amount of space available for the denture resin and teeth due to the need for a bulky, strong, metal substructure. To prevent resin fracturing or the loss of the resin-tooth complex, it is important to attach the resin to the metal using a combination of mechanical and chemical retention. When space is limited, it is often impractical to incorporate sufficient macromechanical retention. The use of chemical retention systems is an asset in these circumstances. The Silicoater MD system (Kulzer) has been used routinely to provide chemical resin bonding for all our implant frameworks, with generally good results.
What's the Clinical Relevance?
Having an understanding of bonding systems that are primarily used by laboratories may seem irrelevant to a busy practitioner. However, the systems do have clinical applications that may be advantageous. Being familiar with the process and testing procedures will improve your communication with the laboratory, and help you to choose the best available system. As is the case with the resin bonding systems we use in our practices, it may not be the particular system that is of primary importance, but how it is employed. A high incidence of clinical failure may be indicative of poor laboratory technique, rather than a fundamental flaw in the bonding system. Clinicians should keep the laboratory informed regarding the performance of in-service prostheses.
An intermediary layer can be applied between the resin and metal to improve the attachment or bond of the materials. This laboratory procedure has important clinical implications, although the routine prescription of a bonding system is probably unwarranted at this time. Using the systems involves additional time and expense, which has to be weighed against the potential benefits. However, because there are situations where resin-metal bonding has been shown to be advantageous, it is appropriate to consider its use on an "as needed" basis.
Our experience has been primarily with the Silicoater and Kevloc systems (Kulzer).This article outlines the procedures used to establish the resin-metal bond, and how clinicians can evaluate the laboratory performance of the Silicoater and Kevloc systems. A subsequent article will report on a laboratory study, which examined various factors affecting the bond strength obtained using these systems. Our interest in the performance of these bonding systems arises from observing the clinical failures that occurred in an implant study group over a five year period.15
Chemical Bonding With the Silicoater MD and Kevloc Systems
Silicoating
In 1984, Musil and Tiller reported achieving improved resin-metal bond strengths through Silicoating, which involved a combination of mechanical and chemical retention.13 The original system involved the application of a silica layer to a metal framework pyrolytically, with a subsequent application of a silane coupling agent, followed by the resin. Based on the manufacturer's claims, it was anticipated that the system would provide a superior method of attaching resin to metal for fixed and removable appliances. In vitro studies indicated that:
- Silicoating produced higher bond strengths than adhesive cements.5,6,9,11
- Silicoating was less affected by thermocycling than other bonding systems.10,11
- The bond strength was relatively constant and independent of the resin-metal combination.5-8,12
The clinical results needed to substantiate the manufacturer's claims and support the in vitro studies were lacking in the North American literature, but were reported by Musil and Tiller in the European literature. However, our own clinical experience indicated that we were achieving varied and inconsistent bonding, which was reflected by the fracture of the resin at the resin-metal interface. The Silicoating technique was awkward in terms of the pyrolytic application of the silica layer, the positioning of the prosthesis within the apparatus, and the fact that the process did not produce a discernable bond layer.
Silicoater MD
The manufacturer subsequently altered the system, by introducing a major change in the method used to apply the silica layer to the metal. Essentially, the technique and machinery used to apply the silica layer were simplified. Another key advantage was that a visible bond layer was discernable with this system. The steps required to use the Silicoating and Kevloc systems are listed in Table I.
Surface Pretreatment
Pretreating the surface of the metal prior to using a chemical bonding system, or as an integral step in the bonding process, is controversial.2,6,7,14 Blasting the metal surface with different materials of various grain sizes has produced conflicting results. In general, it appears that pretreating the metal surface to achieve micromechanical retention will increase bond strength values. Blasting the metal surface with aluminum oxide or sand is thought to increase the surface energy at the metal face, and enhance wettability, thereby improving the adhesion of materials to the metal.2
Establishing the Silica Layer
After the metal surface is pretreated to achieve micromechanical retention, it is cleaned with a chemical (Siliclean) before the silica layer is established in the Silicoater MD unit through a process of vitrification. This process binds silica molecules to free bond sites on the metal surface to form a silica-metal layer of very small molecular thickness. The resulting bond is strong and somewhat elastic, which helps to distribute the strains caused by temperature variations and shearing forces over the metal surface, and reduces microleakage.
Binding the Resin
To bind resins to the silica-metal layer, a silane coupling agent is applied to form a bridge layer, followed by the application of an unfilled resin or opaquer resin to protect the chemically unstable intermediary layer. The application of these different materials, which form the intermediary bonding layers, is done in the laboratory. However, the final application of the resin veneer or resin-tooth matrix is done after the clinical confirmation of the tooth set-up for a removable prosthesis, or the trying in of the fixed framework. The intermediary bonding layers must not be altered during this step, and the surface must be cleaned prior to application of the final resin layer. Failing to remove the wax residue prior to processing will completely negate the advantages of using this chemical bonding system.
The Kevloc System
The Kevloc system (Kulzer) is a more recent method of producing a chemical resin-metal bond. As with the Silicoating techniques, pretreatment with microabrasion is used to activate and clean the metal surfaces, and improve micromechanical retention. However, rather than chemically cleaning the blasted surface, a cleaning brush is used to remove loose surface particles. The silica layer is then produced by applying a chemical primer and bonding agent, which is thermally activated with a hot air handpiece. This bond layer is protected with an unfilled resin or opaquer resin layer, similar to the Silicoater systems.
The main difference and potential advantages of the Kevloc system over the Silicoater MD system are primarily its reduced complexity, and the smaller number of steps required to establish the bond layer. In addition:
- Micromechanical pretreatment is accomplished using small size aluminum oxide particles rather than large particle sand. This type of abrasion unit is readily available in the majority of commercial laboratories.
- Chemicals are an additional expense, and their shelf lives may pose a problem. The chemicals used with the Kevloc system have a six-month shelf life, as compared to a six-week shelf life for the chemicals used with the Silicoater MD system. With the Kevloc system, no chemicals are required to clean the metal surface. This reduces the number of chemicals used.
- Heat activation is achieved with hot air, not through flaming or the use of a burning chamber. The apparatus is less technique sensitive, and can be used to reinstate the bond layer on a discrete area for repair purposes. With the Silicoater systems, the resin matrix and denture teeth must all be removed before the bond can be reinstated for a repair of a fractured prosthesis.
The Kevloc system's manufacturer advocates its use for the application of resin facings made with Artglass (Kulzer). Clinically, the system has been used in various situations with favorable results. The manufacturer has reported additional advantages over other systems, including an improvement in bond strength. Although the literature support for this claim is scant, our comparison of the bond strengths achieved with the Silicoater and Kevloc systems in vitro, which will be reported on in a subsequent article, does support this claim.
Evaluating Resin-Metal Bonding Systems
There is a conspicuous lack of clinical data to support the application of these bonding systems in practice. Clinical studies are time consuming and costly, and it is customary to see laboratory results used as a proxy for actual clinical test- ing. However, when the results of laboratory studies are considered, it is imperative to remember that performance under controlled test conditions may not be a valid predictor of clinical performance. Certain considerations may be helpful when interpreting study results.
- What is the method of testing?
A shear test is the more common testing method, and tends to produce failure at the interface rather than in the resin. This manner of failure has often been cited as an indicator of poor performance. Failure at the interface may be deemed to be a fault of the bonding mechanism, because a cohesive failure in the resin would seem to indicate that the bond is not as strong as the resin. However, the shear and tension tests that have been reported in the literature tend to produce strength values that are not significantly different. The manner of failure may be primarily a reflection of the test procedure, and not indicative of bond strength or clinical performance. Standardized testing procedures for testing bond strengths are outlined by the International Standards Organization (ISO),4 which, if followed, would help reduce the variation in bond strength measurements reported in the literature.
- Does the test process simulate clinical conditions?
The complexity of the stresses that occur at the resin-metal interface is decidedly different in the oral cavity than in laboratory test procedures. In the oral cavity, a material is rarely subjected to an increased load to the point of failure. Restorations are primarily subjected to repetitive loads below the failure threshold, and fail due to fatigue. The handling and environment the specimens are tested in may also affect test results. For instance, specimens that are thermocycled may more closely approximate those in an oral environment than samples that are kept on the bench top.
- Was the test process (method) controlled?
In a laboratory study, consistency in materials and methods is required to maintain a standardized test process. A consistency in operator and technique is difficult to achieve even in a controlled laboratory setting, however. Even when the same procedure is used, variation between cases may exist due to variation between operators.16 Variable results, even under controlled conditions, help to explain why clinical performance is often very difficult to judge. The results have to be fairly dramatic to produce a discernible clinical effect, especially if the number of cases is modest.
- What is the effect of the materials?
Bonding results from the combination of the chemical and microretentive aspects of the system being considered. These factors are further influenced by the alloy and resin systems employed. Results can vary not only because of the test methods, but also because of the test materials. The test materials should be identified, and the combinations of resins and metals kept constant, if a comparison between systems is to be made in a specific study.
Although caution is advised in extrapolating laboratory results into clinical performance recommendations, resin-metal bonding systems have the potential to improve the clinical performance of dental prostheses by improving bond strengths. Generally, laboratory studies indicate that the adhesion of resin to metal is improved by using a bonding systems. Our task is to determine whether the laboratory results indicate that one system provides an appreciably better bond strength value over another system.
All systems rely heavily on appropriate laboratory procedures to provide consistent results. An understanding of the bonding mechanism and laboratory procedures will aid clinicians in their evaluation of study results, communication with their laboratory, and choice of system.
Dr. Mazurat is an assistant professor in the department of restorative dentistry, University of Manitoba, Winnipeg, Man.
Dr. Simona Pesun is in private practice in Winnipeg, Man.
Reprint requests to: Dr. Randall D. Mazurat, University of Manitoba, Faculty of Dentistry, Department of Restorative Dentistry, D227-780 Bannatyne Ave., Winnipeg, MB R3E 0W2.
- Henderson, D. and Steffel, V.L. McCracken's Removable Partial Prosthodontics. 6th ed., St. Louis. CV Mosby, 1981.
- Adept Institute. Metal-resin bonding. Adept Report 2:25-40, 1991.
- Hansson, O. The silicoater technique for resin bonded prostheses; clinical and laboratory procedures. Quintessence Internat 20:85-99, 1989.
- International Standards Organization. Proposal for testing bond strencth to metal. ISO 10477/Dam1, 1993.
- Ishijima, T., Caputo, A.A. and Mito, R. Adhesion of resin to casting alloys. J Prosthet Dent 67:445-449, 1992.
- Luthy, H., Marinello, C.P. and Scharer, P. Factors influencing metal-resin tensile bond strengths to filled composites. Dent Mater 6:73-77, 1990.
- Peutzfeldt, A. and Asmussen, E. Silicoating: evaluation of a new method of bonding composite to metal. Scand J Dent Res 96:171-176, 1986.
- Hansson, O. and Moberg, L.E. Evaluation of three silicoating methods for resin-bonded prostheses. Scand J Dent Res 101:243-251, 1993.
- Caeg, C., Leinfelder, K.F., Lacefield, W.R. et al. Effectiveness of a method used in bonding resins to metal. J Prosthet Dent 64:37- 41, 1990.
- Hansson, O. Strength of bond with Compspan Opaque to three sili- coated alloys and titanium. Scand J Dent Res 98:248-256, 1990.
- Ohno, H., Araki, Y. and Sagara, M. The adhesion mechanism of dental adhesive resin to alloy: relationship between Co-Cr alloy surface structure analyzed by ESCA and bonding strength of adhesive resin. Dent Mater 5:46-65, 1986.
- Kolodney, H., Puckett, A.D. and Brown, K. Shear strength of laboratory processed composite resins bonded to a silane - coated nickel chromium - beryllium alloy. J Prosthet Dent 67:419-422, 1992.
- Musil, R. and Tiller, H.J. The adhesion of dental resin to metal surfaces. The Kulzer Silicoater technique. 1st ed., Wehrbeim: Kulzer and Co. Gmbh. pp. 9-53, 1984.
- May, K.B., Russell, M.M., Razzoag, M.E. et al. The shear strength of polymethyl methacrylate bonded to titanium partial denture framework material. J Prosthet Dent 70:410-413, 1993.
- Mazurat, R.D., Pesun, I.J. and Love, W.B. The role of the restorative dentist in the diagnosis and maintenance phases of implant therapy - Part I: Patient selection. J Can Dent Assoc 60:811-813, 1994.
- Van Noort, R., Noroozi, S., Howard, I.C. et al. A critique of bond strength measurements. J Dent 17:61-67, 1989.