Critčres touchant l'utilisation d'un cadre de décision clinique pour les patients malades : hypertension et diabčte sucré
H.J. Lapointe, DDS, PhD, FRCD(C)
J.E. Armstrong, DDS, M.Sc., MRCD(C)
B. Larocque, MD, FRCP(C)
SOMMAIRE
Dans cet article, on présente les critčres cliniques en vue de déterminer le degré de gravité de la maladie chez les patients atteints d'hypertension ou de diabčte sucré. Cet article sert de complément ŕ un autre que les auteurs ont déjŕ publié et qui s'intitule : Un cadre de décision clinique pour les patients malades : la cardiopathie ischémique et les maladies pulmonaires obstructives chroniques.1 L'hypertension et le diabčte sucré sont expliqués en fonction de la pathophysiologie, des facteurs de risque, des manifestations cliniques et du progrčs de la maladie. Cet article permet aux praticiens, d'une part, de classifier les patients suivant le stade de leur hypertension et de leur diabčte sucré et, d'autre part, d'appliquer cette classification au cadre de décision clinique déjŕ établi pour les patients maladesMots clés MeSH: decision making; dental care for chronically ill; diabetes mellitus; hypertension; severity of illness index.
© J Can Dent Assoc 1998; 64:704-9
Cet article a fait l'objet d'une révision par des pairs.
[ Strategic Reserve, Systemic Illness and Loss Of Strategic Reserve | Hypertension | Diabetes Mellitus | Summary]
Strategic Reserve, Systemic Illness and Loss Of Strategic Reserve
Systemic disease may be thought of as an erosion of an organ system's reserve or ability to respond to internal or external stresses. This diminished adaptive capability results in an increased potential for system failure and medical emergencies as the individual is stressed by apprehension or by the physical demands of dental procedures. From this perspective, it is important to know not only what disease the patient has, but also what reserve he or she has left. In a previous article discussing ischemic heart disease and chronic obstructive pulmonary disease, the authors proposed a scale of 1 to 4 to classify the severity of systemic disease. Stages 1 through 4 represent progressively worsening disease and loss of adaptive capability.1 Hypertension and diabetes mellitus are two other common conditions that lead to tissue damage and reduced strategic reserve and lend themselves to similar analysis.
Definition: Hypertension is an elevation in the blood pressure to a level of 140/90 or greater. A diagnosis is not made on the basis of a single measurement but requires confirmation on at least two further measurements at separate times. Further, the reading should be taken after five minutes of rest and using an appropriate cuff and appropriate technique. The importance of the routine measurement of blood pressure cannot be overemphasized. Blood pressure measurement in the dental office is an effective screening tool that alerts patient, dentist and physician to an unsuspected potential problem.2
Incidence and Risk Factors: Hypertension is an extremely common disorder. In a relatively recent article describing the 20 most commonly prescribed drugs, 8 of the 20 were drugs that are given for hypertension or its effects on end organ systems.3 Overall, hypertension affects 20% of white North Americans and 30% of black North Americans 18 years of age or older. As patients age, the prevalence increases, going up to 64% of people between the ages of 64 and 74.4 In addition to race and increasing age, obesity and increased salt intake put patients at increased risk of hypertension.5
Pathology: Fewer than 5% of hypertensive patients have hypertension secondary to an identifiable cause such as renal disease, adrenocortical hyperfunction, pheochromocytoma or thyrotoxicosis. The remainder have essential hypertension, which has no identifiable etiology; however, there is recognized to be a failure in the regulation of vascular resistance. In the long term, hypertension results in arterial damage, which leads to end organ damage in areas such as the heart, retina, kidneys and brain.2
Clinical Manifestations: In many patients there is no clinical manifestation of hypertension other than an increase in the measured blood pressure. This increase may persist for many years before other clinical signs or symptoms occur. Usually, clinical signs and symptoms of hypertension are an indication of vascular damage in end organs such as the retina or the heart. Early symptoms include occipital headache, vision changes, ringing in the ears, dizziness, weakness and tingling of the hands and feet. Progression of the disease can result in congestive heart failure, stroke, ischemic heart disease (angina or MI), renal failure or blindness.2 Hypertension is the key risk factor for atherosclerotic coronary artery disease, accounting for 35% to 45% of annual cardiovascular morbidity and mortality. The greatest risk of hypertension-associated coronary complications is concentrated in patients with hypercholesterolemia, impaired glucose tolerance or left ventricular hypertrophy and in patients who smoke.4
It is the manifestations of end organ damage that are of concern in the dental management of patients with hypertension. Stroke and myocardial infarction brought on by the stress of a procedure are two of the potential acute manifestations of hypertension that we may see in the dental setting.
Disease Classification By Blood Pressure Measurement: Elevation in blood pressure is categorized from high-normal to severe based on measurement. Both the systolic and the diastolic readings must be taken into account by the physician making the diagnosis (Table I).2,6
Disease Classification By Complexity Of Pharmacology: In the management of hypertension, a staged or stepped approach to pharmacological management is recommended. As hypertension worsens or proves resistant to therapy, the drugs used to treat it may be increased in dose, changed or increased in number. Careful analysis of the patient's list of drugs usually indicates the medical diagnosis, and analysis of changes in therapy helps to determine the level of severity (Table II).6
When therapy is successful, it is recommended that effort be made to decrease the number and dose of medications to a minimal maintenance level. Reduction is most effective in patients who continue to follow non-pharmacologic therapeutic recommendations, such as regular exercise, weight loss, salt restriction, moderation of alcohol intake and cessation of smoking.6 In reality, most patients stay on lifelong therapy to maintain control.4
Level Of Risk and Procedural Complexity: In any clinical situation, the systemic disease state of the patient must be assessed along with the procedural complexity and the relative risk of complications. In the case of hypertension, previously undiagnosed or poorly controlled hypertension should trigger a referral back to the physician for further assessment and possible initiation or modification of antihypertensive therapy.
Definition: Diabetes mellitus is a diverse group of disorders that produce hyperglycemia as a prominent manifestation, ultimately as a function of the inability to secrete enough insulin to meet metabolic needs. The two most common forms of this disease are Type I diabetes and Type II diabetes.7
Type I accounts for approximately 25% of patients with diabetes; its onset is most commonly seen in childhood or young adulthood. It is caused by immune-mediated destruction of the insulin-producing beta islet cells of the pancreas. The destruction of these cells leads to almost total loss of production of endogenous insulin. For patients with Type I diabetes, insulin injection is required to regulate glucose levels and prevent diabetic ketoacidosis.
Type II accounts for approximately 75% of patients with diabetes; its onset is usually after age 40. Patients with Type II diabetes produce insulin; however, there may be inadequate production or resistance to its action. These patients are not ketosis prone. Type II diabetes may be managed by diet and weight control, oral hypoglycemics or insulin to regulate glucose levels.7,8
Incidence and Risk Factors: It is estimated that 2% to 4% of North Americans have diabetes mellitus. Auto-immune reactions, possibly triggered by viral illness (such as rubella or cytomegalovirus), are causative in the development of Type I diabetes. Although both Type I and Type II diabetes have genetic components, genetics are a greater factor in Type II. In addition to genetics, obesity has a poorly understood but important role in the development of Type II diabetes.9
Pathology: The primary defect in Type I diabetes is immune-mediated destruction of the insulin-producing pancreatic islet cells. The destruction of these cells leads to an absolute deficiency of insulin. In contrast, the patient with Type II diabetes continues to produce insulin in variable amounts. In addition to reduced insulin (in some cases), the defect in Type II diabetes appears to lie in a reduction in insulin receptors and reduced post-receptor activity.9 In a patient with either type of untreated diabetes, the relative lack of insulin results in hyperglycemia combined with an inability to use glucose. In the patient with Type I diabetes, this combination can lead to potentially life-threatening diabetic ketoacidosis.
The long-term implication of diabetes is the development of vascular complications secondary to microangiopathy and accelerated atherosclerosis. These complications usually start to occur 15 to 20 years after the initial diagnosis.8 The vascular complications lead to complications in various organ systems, most notably the kidneys, the heart, the peripheral vascular system and the eyes.7
Clinical Manifestations: The classic triad of polydipsia, polyphagia and polyuria seen in acute Type I diabetes is secondary to hyperglycemia combined with an inability to metabolize glucose. This combination leads to the metabolizing of fat stores and the development of ketoacidosis. It is very uncommon for a diabetic patient to present in a dentist's office in this condition. The patient at that stage is usually quite ill and is far more likely to be seen by the family physician or in the emergency room. In contrast, the dental practitioner frequently has the opportunity to manage the dental problems of the patient with diagnosed diabetes.9
Disease Classification By Clinical Symptomatology: Even when diabetes is well controlled, patients present with long-term manifestations of the underlying disease. The clinical signs and symptoms of the patient with diagnosed diabetes are either due to problems with control of the underlying diabetes or are associated with other systemic disease secondary to the microangiopathy and atherosclerosis associated with long-standing diabetes (Tables III and IV).7
| Table III | ||||||||||||||||
| Diabetes — Disease Classification by Clinical Symptomatology Associated with Control of Diagnosed Diabetes | ||||||||||||||||
|
||||||||||||||||
| Table IV | ||||||||
| Diabetes — Disease Classification by Clinical Symptomatology of Systemic Disease Secondary to Diabetes | ||||||||
|
Disease Classification By Complexity Of Pharmacology: The control of hyperglycemia associated with diabetes and the avoidance of hypoglycemia as a result of medication overdose, inadequate caloric intake or excess exercise require careful monitoring and balance of therapy. In the patient with Type I diabetes, management absolutely requires exogenous insulin. In the patient with Type II diabetes, therapy may range from weight and diet control to individual or combination oral hypoglycemics, with or without insulin. All of these therapies require careful monitoring of blood glucose levels to avoid extremes in serum glucose as well as to minimize the long-term systemic complications of diabetes (Tables V and VI).7,8
| Table V | ||||||||
| Type I Diabetes — Disease Classification by Complexity of Pharmacology | ||||||||
|
| Table VI | ||||||||||
| Type II Diabetes — Disease Classification by Complexity of Pharmacology | ||||||||||
|
||||||||||
The dental practitioner must be aware of the potential for acute problems associated with the underlying disease (hyperglycemia and hypoglycemia) or its systemic manifestations (ischemic heart disease, peripheral vascular disease, etc.) or both. In addition, the practitioner must be alert to the fact that dental treatment may cause disruptions in the patient's balance between caloric intake and insulin or oral hypoglycemic therapy. This disruption has the potential to lead to an acute hypoglycemic episode, which can be a life-threatening medical emergency. Precautions such as early morning appointments and advising the patient to take her or his normal medications and meals help prevent such complications in the ambulatory setting.9
Procedural Stress: The prevention of systemic complications requires the maintenance of a careful balance between the stress of the procedure and the patient's ability to cope with that stress. The ability to maintain this balance is predicated on careful analysis of the patient's systemic reserve (as suggested on a scale of 1 to 4) as well as an understanding of the stresses involved in various procedures. As in the authors' previous publication, a simple classification of procedures is presented for the purposes of assessing the balance between systemic disease and procedural stress (Table VII).1 Please note that patient anxiety may increase the stress to the patient and must be considered as part of the analysis.
| Table VII | ||||||||
| Classification of Procedural Stress | ||||||||
|
|
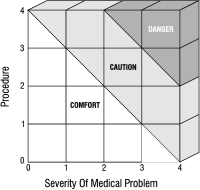
| Fig. 1: Correlation of medical compromise with procedural stress: A grid system is used to plot the severity of the patient's medical problems (horizontal axis) against the anticipated stress of the proposed procedure (vertical axis). The point at which these two intersect falls within the comfort, caution or danger zone of the practitioner. |
Determination Of Relative Risk and Treatment Planning: Disease severity and risk can be correlated using the proposed grid system. Disease severity from 0 to 4 is plotted on the horizontal axis, and procedural stress from 0 to 4 is plotted on the vertical axis (Fig. 1). The positions and slopes of the lines that divide comfort, caution and danger zones vary from clinician to clinician and, for a given clinician, from situation to situation. These variances depend on:
1. the clinician's training and experience with the proposed procedure;
2. the clinician's familiarity with the systemic disease and its implications;
3. the procedural complexity;
4. the severity of the disease;
5. the facilities and equipment available;
6. the urgency or emergency of the proposed treatment.
Should a given procedure in a given patient exceed the practitioner's comfort or caution levels, then modification of treatment plan or referral to a physician or specialist may be warranted.1
This article has proposed clinical criteria for the classification, on a scale of 1 to 4, of loss of systemic reserve for patients with hypertension or diabetes mellitus. These criteria complement the clinical criteria for ischemic heart disease and chronic obstructive pulmonary disease proposed in a previous article.1 The criteria allow practitioners to use a clinical decision-making framework to correlate medical risk to procedural complexity and express the relative risk in terms of the practitioner's comfort and caution levels. The framework then enables the practitioner to make more objective clinical decisions on treatment modification or referral. As with all guidelines of this nature, individual patients must be assessed on their own individual presentations. The risks of treatment must be reassessed at each future encounter.
Dr. Lapointe is associate professor and chair, Division of Oral and Maxillofacial Surgery and Hospital Dentistry, Faculty of Dentistry, University of Western Ontario; and chief of dentistry, Department of Dentistry, St. Joseph's Health Centre.
Dr. Armstrong is clinical assistant professor, Division of Oral and Maxillofacial Surgery and Hospital Dentistry, Faculty of Dentistry, University of Western Ontario; and chief of dentistry, Department of Dentistry, London Health Sciences Centre.
Dr. Larocque is associate professor, Department of Medicine, St. Joseph's Health Centre and Faculty of Medicine, University of Western Ontario.
Reprint requests to: Dr. H.J. Lapointe, Division of Oral and Maxillofacial Surgery, Faculty of Dentistry, University of Western Ontario, London, ON N6A 5C1.
References
1. Lapointe HJ, Armstrong JE, Larocque B. A clinical decision-making framework for the medically compromised patient: ischemic heart disease and chronic obstructive pulmonary disease. J Can Dent Assoc 1997; 63:510-6.
2. Little JW, Falace DA. Hypertension. In: Dental management of the medically compromised patient. 4th ed. St Louis: Mosby; 1993. p. 161-74.
3. Desjardins PJ. The top 20 prescription drugs and how they affect your dental practice. Compend Contin Educ Dent 1992; 13:740-54.
4. Rosamund TL, Fields LE. Hypertension. In: Manual of medical therapeutics. 26th ed. Toronto: Little, Brown and Company; 1989. p. 72-89.
5. Williams GH. Hypertensive vascular diseases. In: Isselbacher KJ et al., editors. Harrison's principles of internal medicine. 13th ed. (on CD-ROM) New York: McGraw-Hill; 1996 (Chapter 209, Section 2, Part 7).
6. Joint National Committee on Prevention, Detection, Evaluation and Treatment of High Blood Pressure. The sixth report of the Joint National Committee on Prevention, Detection, Evaluation and Treatment of High Blood Pressure. Bethesda, MD: U.S. Department of Health and Human Services; NIH publication No. 98-4080; 1997.
7. Orland MJ. Diabetes Mellitus. In: Isselbacher KJ et al., editors. Harrison's principles of internal medicine. 13th ed. (on CD-ROM) New York: McGraw-Hill; 1996 (Chapter 337, Section 1, Part 13).
8. Foster DW. Diabetes Mellitus. In: Isselbacher KJ et al., editors. Harrison's principles of internal medicine. 13th ed. (on CD-ROM) New York: McGraw-Hill; 1996 (Chapter 337, Section 1, Part 13).
9. Little JW, Falace DA. Diabetes. In: Dental management of the medically compromised patient. 4th ed. St. Louis: Mosby; 1993. p. 341-60.